Annual Report 2023
Department of Breast Surgery
Akihiko Suto, Shin Takayama, Takeshi Murata, Chikashi Watase, Hinako Maeda, Ayumi Ogawa, Hiromi Hashiguchi
Introduction
The Department of Breast Surgery mainly deals with surgical treatment of breast cancer, as well as diagnosis of breast diseases, postoperative adjuvant endocrine therapy and surveillance after surgery. In fiscal 2023, we performed a total of 744 operations on breast diseases (697 were primary breast cancer, Table 1, Table 2).
Breast conserving surgery such as breast partial resection (Bp) or Radiofrequency Ablation (RFA) accounted for 29% (219 of 744) of total breast surgeries in our department in 2023, and the breast conserving rate has been constant in recent years. On the other hand, the rate of immediate reconstruction surgeries has gradually increased. One of the reasons is the increasing need of patients for immediate reconstruction surgeries. In our hospital, since 2010, immediate breast reconstruction has become one of the choices for patients for whom breast preservation is cosmetically difficult, and a total of 133 immediate breast reconstructions were performed in fiscal 2023 comprising 29% of all mastectomies. 25 of 133 were tissue expander (TE) insertions, and 108 autologous reconstructions (97 DIEP: deep inferior epigastric perforator flap; 11 LD: latissimus dorsi muscle flap) were performed (Table 3). In 2018, since Breast Implant-Associated Anaplastic Large Cell Lymphoma (BIA-ALCL) was reported overseas, implant reconstruction significantly decreased, and the rate of autologous tissue reconstruction increased. We perform these reconstruction surgeries in cooperation with plastic surgeons depending on patients' needs.
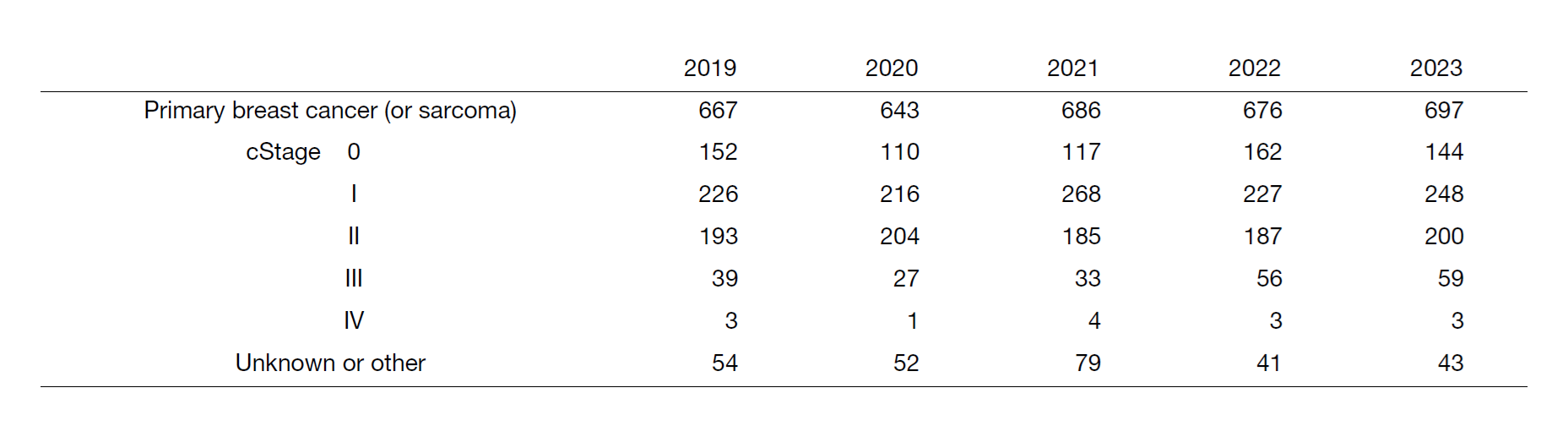
Table 2. Type of procedure (breast surgery)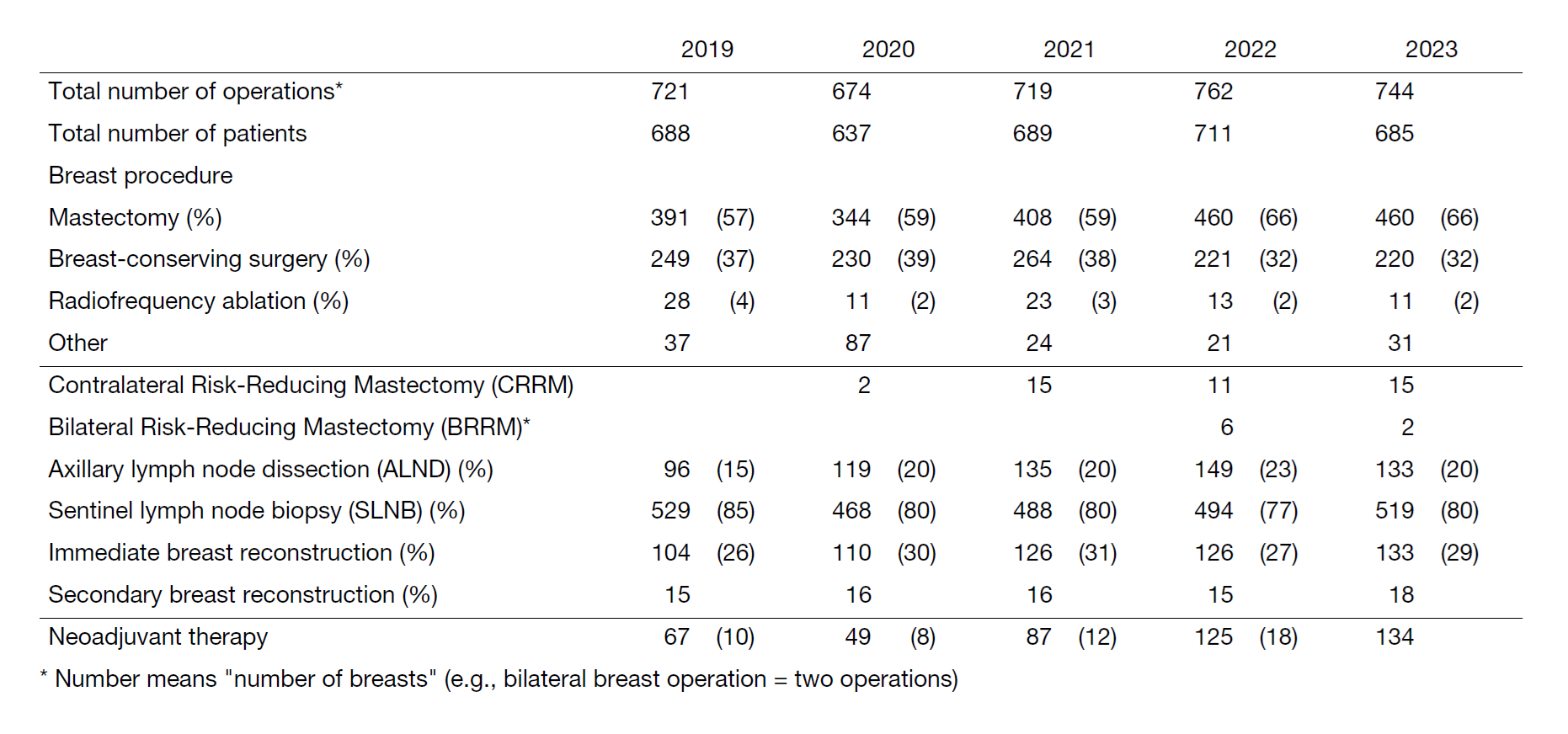

Table 3. Type of procedure (reconstruction surgery)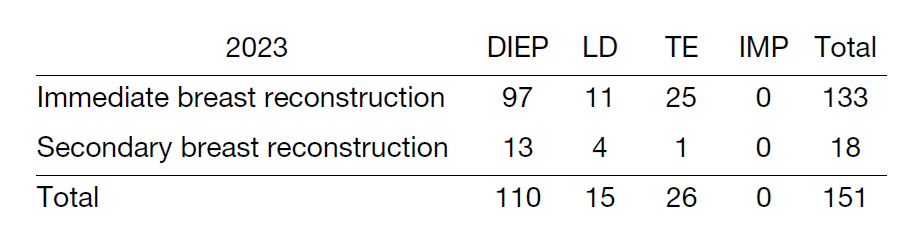

The new less-invasive technique, RFA, is one of the topics of our surgeries. RFA is a new treatment that ablates tumors using electro-radio waves. The advantages of RFA include reduced physical burden on the patient, lower morbidity, lower operating time and avoiding breast deformation after surgery. Recently, RFA has become one of the standard treatment choices for early breast cancer, and in fiscal 2023, 11 RFAs were performed in our hospital. We also started performing single port endoscopic nipple-sparing mastectomy (E-NSM) for early breast cancer, and in fiscal 2023, 9 E-NSMs were performed in our hospital.
We also focus on extended surgery. For example, for ulcerating breast cancer with distant metastasis and bulky breast cancer judged to be unresectable at another hospital, we perform palliative breast resection with or without reconstruction as much as possible for the purpose of local control. We performed 2 salvage surgeries in fiscal 2023. We are actively working to improve not only the patient's survival but also the patient's QOL.
Furthermore, we also started working on management of hereditary breast cancer and ovarian cancer syndrome (HBOC) in 2020. Many patients had prior genetic counseling and then took the genetic testing. Some of them underwent the contralateral risk-reducing mastectomy (CRRM). In 2023, a total of 17 cases had CRRM. Genetic specialists and gynecologists manage patients with HBOC to meet their needs. As mentioned above, we engage in various activities to meet the diverse needs of patients with breast cancer.
The Team and What We Do
Our department is comprised of six staff surgeons specialized in breast cancer (Dr. Takayama, Dr. Murata, Dr. Watase, Dr. Maeda, and Dr. Ogawa), one chief resident (Dr. Hashiguchi), and two or three rotating residents. From 8:00 every morning, all the staff and residents perform in-patient rounds together. Weekly pre-operative and neo-adjuvant conferences are held on Mondays from 17:00 to 18:30. At the conferences, we share discussions with surgeons, and the diagnostic images are reviewed for every pre-operative patient. Every Friday from 7:45 to 8:15, we hold a journal club and share the most up-to-date knowledge on breast oncology. A breast pathology/ imaging conference is held on the second Wednesday every two months from 18:00 to 19:00 to discuss problems with diagnostic imaging, as well as pathologically interesting cases. A conference about studies, institutional treatment guidelines, and recent topics regarding breast cancer is also held irregularly by a multidisciplinary team. Treatment guidelines for primary and metastatic breast cancer have been regularly updated through this multidisciplinary discussion since 2003.
We perform surgeries from Monday to Friday; there are usually 14 to 16 cases of breast cancer in a week. Table 1 shows the total number of patients with primary breast cancer (including breast primary sarcoma) and other breast diseases. The types and number of operative procedures are shown in Table 2.
Research Activities
1. A multicenter study on learning and diagnostic accuracy of breast ultrasound imaging by Artificial Intelligence.
2. A study on the construction of a prediction model for postoperative prognosis of breast cancer by machine learning using Japanese patients' data.
3. Metabolome analysis for breast cancer patients with neoadjuvant chemotherapy.
4. A study on the prognostic impact of progesterone receptor status of isolated locoregional recurrence of breast cancer.
5. A study on the prognostic importance of progesterone receptor-low-positive status in pre- and post-menopausal breast cancer patients.
Clinical Trials
1. Patients offered Radio Radiofrequency ablation therapy for early breast cancer as local therapy (PO-RAFAELO study)
2. Intensive versus standard post-operative surveillance in high risk breast cancer patients (JCOG1204, INSPIRE Trial)
3. Single-arm confirmatory trial of endocrine therapy alone for estrogen positive, low-risk ductal carcinoma in situ of the breast (Low-risk DCIS with endocrine therapy alone-TAM) (JCOG1505, LORETTA Trial)
4. Avoid Mastectomy Using Trastuzumab, Pertuzumab and Radiation Study for Breast Cancer (JCOG1806, AMATERAS-BC)
5. A multicenter, randomized, open-label phase III study comparing T-DXd and T-DM1 in high-risk HER2-positive breast cancer patients with residual invasive lesions in the breast or axillary lymph nodes after postoperative therapy (DESTINY-Breast05)
6. Asian multicenter prospective study in HER2 positive early breast cancer for detecting minimal residual disease by circulating tumor DNA analysis with neoadjuvant chemotherapy (HARMONY study)
7. Feasibility study on the safety and efficacy of a new axillary reduction surgery (tailored axillary surgery, TAS) in patients with axillary lymph node-positive primary breast cancer
Future Prospects
The aims of our activities are as follows:
1. Clinical activities
To provide the very best breast surgical treatment
2. Research activities
To develop less invasive breast surgical procedures
3. Educational activities
To train specialists in breast cancer who will lead the future of cancer fields.
List of papers published in 2023
Journal
1. Akechi T, Furukawa TA, Noma H, Iwata H, Toyama T, Higaki K, Matsuoka H, Zenda S, Iwatani T, Akahane K, Inoue A, Sagara Y, Uchida M, Imai F, Momino K, Imaizumi G, Yamaguchi T, Mashiko T, Miyaji T, Horikoshi M, Sakurai N, Onishi T, Kanemitsu Y, Murata T, Wanifuchi-Endo Y, Kuroda H, Nishikawa R, Miyashita M, Abe M, Uchitomi Y. Optimizing smartphone psychotherapy for depressive symptoms in patients with cancer: Multiphase optimization strategy using a decentralized multicenter randomized clinical trial (J-SUPPORT 2001 Study). Psychiatry and clinical neurosciences, 78:353-361, 2024
2. Matsuzaki J, Kato K, Oono K, Tsuchiya N, Sudo K, Shimomura A, Tamura K, Shiino S, Kinoshita T, Daiko H, Wada T, Katai H, Ochiai H, Kanemitsu Y, Takamaru H, Abe S, Saito Y, Boku N, Kondo S, Ueno H, Okusaka T, Shimada K, Ohe Y, Asakura K, Yoshida Y, Watanabe SI, Asano N, Kawai A, Ohno M, Narita Y, Ishikawa M, Kato T, Fujimoto H, Niida S, Sakamoto H, Takizawa S, Akiba T, Okanohara D, Shiraishi K, Kohno T, Takeshita F, Nakagama H, Ota N, Ochiya T. Prediction of tissue-of-origin of early stage cancers using serum miRNomes. JNCI cancer spectrum, 7:pkac080, 2023
3. Maseki H, Jimbo K, Watase C, Murata T, Shiino S, Takayama S, Yamamoto N, Satomi K, Maeshima A, Yoshida M, Suto A. Clinical significance of tumor cell seeding associated with needle biopsy in patients with breast cancer. Asian journal of surgery, 46:3700-3704, 2023
4. Murata T, Yoshida M, Shiino S, Ogawa A, Watase C, Satomi K, Jimbo K, Maeshima A, Iwamoto E, Takayama S, Suto A. A prediction model for distant metastasis after isolated locoregional recurrence of breast cancer. Breast cancer research and treatment, 199:57-66, 2023
5. Yamauchi H, Toi M, Takayama S, Nakamura S, Takano T, Cui K, Campbell C, De Vos L, Geyer C Jr, Tutt A. Adjuvant olaparib in the subset of patients from Japan with BRCA1- or BRCA2-mutated high-risk early breast cancer from the phase 3 OlympiA trial. Breast cancer (Tokyo, Japan), 30:596-605, 2023
6. Sanomachi T, Okuma HS, Kitadai R, Kawachi A, Yazaki S, Tokura M, Arakaki M, Saito A, Kita S, Yamamoto K, Maejima A, Kojima Y, Nishikawa T, Sudo K, Shimoi T, Noguchi E, Fujiwara Y, Sugino H, Shiino S, Suto A, Yoshida M, Yonemori K. Low HER2 expression is a predictor of poor prognosis in stage I triple-negative breast cancer. Frontiers in oncology, 13:1157789, 2023
7. Murata T, Yoshida M, Shiino S, Watase C, Ogawa A, Shikata S, Hashiguchi H, Yoshii Y, Sugino H, Jimbo K, Maeshima A, Iwamoto E, Takayama S, Suto A. Assessment of nuclear grade-based recurrence risk classification in patients with hormone receptor-positive, human epidermal growth factor receptor 2-negative, node-positive high-risk early breast cancer. Breast cancer (Tokyo, Japan), 30:1054-1064, 2023
8. Miyakoshi J, Yazaki S, Shimoi T, Onishi M, Saito A, Kita S, Yamamoto K, Kojima Y, Sumiyoshi-Okuma H, Nishikawa T, Sudo K, Noguchi E, Murata T, Shiino S, Takayama S, Suto A, Fujiwara Y, Yoshida M, Yonemori K. Discordance in PD-L1 expression using 22C3 and SP142 assays between primary and metastatic triple-negative breast cancer. Virchows Archiv, 483:855-863, 2023
9. Sasada S, Kondo N, Hashimoto H, Takahashi Y, Terata K, Kida K, Sagara Y, Ueno T, Anan K, Suto A, Kanbayashi C, Takahashi M, Nakamura R, Ishiba T, Tsuneizumi M, Nishimura S, Naito Y, Hara F, Shien T, Iwata H. Prognostic impact of adjuvant endocrine therapy for estrogen receptor-positive and HER2-negative T1a/bN0M0 breast cancer. Breast cancer research and treatment, 202:473-483, 2023
10. Shiino S, Tokura M, Nakayama J, Yoshida M, Suto A, Yamamoto Y. Investigation of Tumor Heterogeneity Using Integrated Single-Cell RNA Sequence Analysis to Focus on Genes Related to Breast Cancer-, EMT-, CSC-, and Metastasis-Related Markers in Patients with HER2-Positive Breast Cancer. Cells, 12:2286, 2023
11. Takayama S, Kinoshita T, Shiino S, Jimbo K, Watanabe KI, Fujisawa T, Yamamoto N, Onishi T, Shien T, Ito M, Takahashi M, Futamura M, Aruga T, Kaneko K, Suto A. Patients Offer Radiofrequency Ablation Therapy for Early Breast Cancer as Local Therapy (PO-RAFAELO) Study under the Patient-proposed Health Services. JMA journal, 6:505-512, 2023
12. Shikata S, Murata T, Yoshida M, Hashiguchi H, Yoshii Y, Ogawa A, Watase C, Shiino S, Sugino H, Jimbo K, Maeshima A, Iwamoto E, Takayama S, Suto A. Prognostic impact of HER2-low positivity in patients with HR-positive, HER2-negative, node-positive early breast cancer. Scientific reports, 13:19669, 2023
