Annual Report 2024
Department of Thoracic Surgery
Masahiro Tsuboi, Keiju Aokage, Tomohiro Miyoshi, Kenta Tane, Yuuki Matsumura, Joji Samejima, Makoto Tada
Introduction
The Department of Thoracic Surgery has three core missions: surgical treatment, surgical resident training, and clinical research. Our thoracic surgeries focus on treating thoracic neoplasms, including primary and metastatic lung tumors, as well as mediastinal, pleural, and chest wall tumors. The department specializes in the surgical management of pulmonary carcinomas.
Routine surgical procedures for carcinoma include limited resections (wedge or segmental resection) and standard resections (lobectomy or pneumonectomy), performed with or without systematic lymph node dissection. Thoracoscopic assistance is utilized in nearly all cases. Additionally, robotic-assisted thoracic surgery and single-port thoracoscopic surgery are part of our surgical repertoire.
Non-routine surgical interventions involve advanced techniques such as broncho-/angio-plasty, combined resections with adjacent structures, and perioperative adjuvant treatments.
Since its establishment in 1992, the department has been a leading contributor to lung cancer treatment and research in Japan. It has also actively participated in international and national scientific forums. This year alone, the department published 11 scientific papers in English and delivered 48 presentations: 14 at international conferences, 30 at national meetings, and four at regional events.
The Team and What We Do
The Department of Thoracic Surgery currently comprises four consultant surgeons, including a chief, and eight or nine residents. Our department employs a team-based approach to both patient care and resident training. Every Tuesday evening, potential surgical cases are presented at a multidisciplinary team conference attended by thoracic surgeons, oncology physicians, radiologists, and residents. Each case is meticulously reviewed and discussed. To enhance English proficiency among staff and residents, discussions on treatment modalities are conducted in English. This practice also facilitates the involvement of visiting physicians from other countries and prepares our team for international presentations. Additionally, selected patients' records undergo radiological and cytopathological review every Friday morning. These reviews are intended to enhance the correlation between radiological and pathological findings, accurately assess surgical indications, and deepen knowledge of rare histological types. Case review meetings are held twice a week by a multidisciplinary team: on Tuesdays for resectable or borderline resectable diseases, and on Wednesdays for unresectable or metastatic diseases. We believe these activities contribute significantly to advancing knowledge, refining treatment indications, and improving surgical outcomes.
For non-small cell lung cancer, surgical resection is indicated as a curative treatment for primary pulmonary carcinomas in clinical stages I, II, and IIIA without bulky or multistation mediastinal lymph node involvement. Similarly, primary pulmonary small cell carcinomas in clinical stage I are candidates for surgical resection. For cases with bulky or clinically and histologically confirmed multistation mediastinal lymph node metastases, invasion of neighboring vital structures, or small cell cancers in clinical stage II and later, optimal treatment modalities are being actively explored through clinical trials to improve the poor prognosis associated with these conditions.
Resection of metastatic lung tumors is performed according to the modified Thomford criteria, with decisions made after thorough consultation with patients. The majority of these cases involve metastases from colorectal carcinoma, while thymic epithelial tumors account for most mediastinal tumor cases.
The surgical procedures in our department have remained largely consistent over the past decade. However, the adoption of port-access thoracoscopic surgery has increased significantly in recent years. Approximately 20% of our surgeries are now completed via a three-port approach, while 70% are video-thoracoscopically assisted.
Postoperative hospital stays have steadily decreased, with three days being the shortest recorded stay and a median of seven days for primary lung cancer cases. These shorter stays are achieved alongside a slightly improved complication rate compared to standard benchmarks. This year, 30-day operative mortality occurred in two patients undergoing surgery for primary lung cancer.
Research Activities
Our research mission is to cure as many patients with lung cancer and other thoracic malignancies as possible, while preserving their quality of life. To achieve this, we focus on initiatives uniquely suited to the National Cancer Center's capabilities and take a leading role in multi-center and multinational research collaborations.
Research in the field of combined treatment, particularly immunotherapy and molecular targeted therapy, has progressed to clinical trials. Some of these treatments have already been approved and reimbursed as standard therapies. Our department aims to deepen the understanding of the cellular and molecular mechanisms driving lung cancer development and progression, translating these insights into innovative immunotherapy-based prevention and treatment strategies.
Recently, alongside ongoing research on surgical techniques and perioperative care, we have expanded our efforts to include the development of medical devices, further contributing to advancements in patient care and treatment outcomes.
Clinical Trials
Major ongoing clinical trials are as follows:
1. JCOG0802/WJOG4607: Phase III study of lobectomy versus sublobar resection (segmentectomy) for peripheral small-area non-small cell lung cancer (NSCLC).
2. JCOG1211: Non-randomized confirmatory study of sublobar resection for clinical T1N0 lung cancer with predominantly ground-glass opacity.
3. JCOG1205/1206: Phase III study of adjuvant chemotherapy for high-grade neuroendocrine lung cancer.
4. JCOG1710A: Prospective observational study evaluating ADL outcomes in elderly lung cancer surgery patients.
5. JCOG1413: Randomized controlled trial of selective lymphadenectomy for clinical stage I/II NSCLC.
6. JCOG1708: Phase III randomized controlled trial of sublobar resection for clinical stage I NSCLC with idiopathic pulmonary fibrosis (IPF).
7. JCOG1807C: Single-arm confirmatory study of multidisciplinary treatment, combining durvalumab pre- and postoperatively after chemoradiotherapy for apical chest wall invasive cancer.
8. JCOG1906: Single-arm confirmatory study of follow-up for early-stage lung cancer based on chest CT scan findings.
9. JCOG1916: Phase III randomized controlled study of postoperative radiotherapy for pathological N2 NSCLC.
10. JCOG2012: Randomized controlled study of postoperative surveillance for pathological stage II-IIIA NSCLC.
11. JCOG1909: Randomized controlled study of segmentectomy vs. wedge resection for lobectomy-treated high-risk clinical stage IA NSCLC.
12. JCOG2103: Phase III randomized trial verifying the therapeutic value of primary tumor resection for clinical stage IVA (cT1-2bN0-1M1a) NSCLC with pleural dissemination difficult to diagnose on imaging.
13. JCOG2217: Randomized controlled trial of lobectomy versus segmentectomy for non-small cell lung cancer (>2-3 cm) with solid components and ground-glass opacities.
14. JCOG2109: Randomized controlled trial of segmentectomy versus wedge resection for small peripheral NSCLC in patients aged 80 or older.
15. JCOG0707A1: Ancillary study of phase III clinical trial of postoperative chemotherapy for resected pathological stage I (T1 > 2 cm) NSCLC.
16. WJOG17123L: A multicenter prospective observational study investigating postoperative adjuvant therapy for pathological stage IA2-IIA EGFR mutation-positive non-small cell lung cancer.
17. PV STUDY: A multicenter randomized controlled trial investigating heparin administration to prevent pulmonary vein stump thrombosis after left-sided pneumonectomy.
18. Study on ALK staining: Comprehensive study on ALK staining in completely resected cases of pathological stage IA1-IIIB lung adenocarcinoma.
19. Biomarker research: Whole genome analysis biomarker research in surgical cases of non-small cell lung cancer.
20. Atezolizumab study: Prospective multicenter observational study of postoperative adjuvant therapy with atezolizumab for resected non-small cell lung cancer.
21. Malignant pleural mesothelioma study: Examination of the usefulness of curative surgery for malignant pleural mesothelioma in Japan using NCD data, Joint Committee on Lung Cancer Registries' 12th project.
22. 3D reconstruction study: Multicenter study on constructing 3D reconstruction images based on non-contrast chest CT scans.
23. Pirfenidone study: Phase III study on perioperative pirfenidone therapy to suppress postoperative acute exacerbation in patients with NSCLC complicated by idiopathic pulmonary fibrosis (IPF).
24. STOP AIR study: Observational study predicting persistent pulmonary fistula using a digital drainage system.
25. Biomarker exploratory study: Phase II clinical trial of induction therapy with pembrolizumab + ramucirumab and multidisciplinary treatment for PD-L1-positive stage IB-IIIA NSCLC.
26. JIPANG study: Postoperative adjuvant chemotherapy for pathological stage II-IIIA non-squamous NSCLC, Phase III study, advanced medical care B.
27. East Energy study: Phase II clinical trial of induction therapy with pembrolizumab + ramucirumab and surgery for PD-L1-positive stage IB-IIIA NSCLC.
28. POTENTIAL study: Observational study of stage I NSCLC patients at high risk of recurrence treated with preoperative nivolumab.
Education
Our training program is designed to educate residents by enhancing their knowledge and technical skills in the treatment of lung cancer, other thoracic malignancies, and benign tumors such as hamartomas and mediastinal cystic lesions. Additionally, we aim to foster in trainees a commitment to continuous self-reflection and lifelong learning, as well as the ability to communicate openly with all healthcare providers while upholding a respectful and professional demeanor.
Future Prospects
Significant progress has been made in the treatment of thoracic malignancies, including lung cancer, mesothelioma, thymic malignancies, and lung metastases, driven by advancements in molecular targeted therapies and immune checkpoint inhibitors. However, perioperative treatment strategies remain in an exploratory phase.
Our research and development efforts in surgical techniques continue to prioritize both oncological effectiveness and minimally invasive approaches. The integration of our laboratory's activities with clinical research is crucial for advancing treatment and improving post-surgical cure rates.
We remain committed to delivering effective treatments to patients with thoracic cancers as swiftly as possible, collaborating closely with researchers and companies in Japan and worldwide.
Table 1. Number of patients with thoracic surgery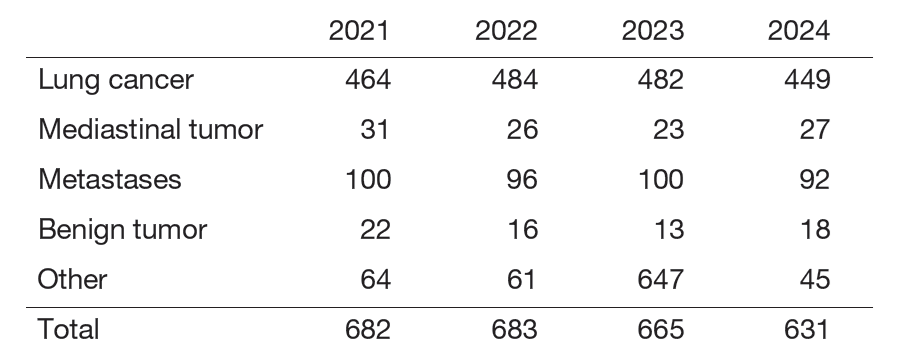

Table 2. Type of procedure in surgical cases with primary lung cancer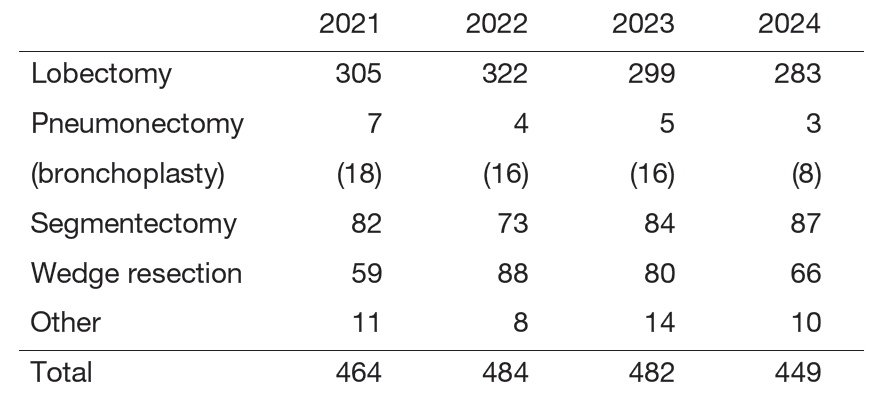

List of papers published in 2024
Journal
1. Miyoshi T, Tsuboi M. Postoperative adjuvant therapy with molecularly targeted agents for non-small cell lung cancer. International journal of clinical oncology, 30:210-214, 2025
2. Onodera K, Aokage K, Wakabayashi M, Ikeno T, Morita T, Ohashi S, Miyoshi T, Tane K, Samejima J, Tsuboi M. An accurate prediction of negative lymph node metastasis with consideration of glucose metabolism in early-stage non-small cell lung cancer. General thoracic and cardiovascular surgery, 72:24-30, 2024
3. Miyoshi T, Tane K, Samejima J, Aokage K, Tsuboi M. Predictors of residual simultaneous multiple ground-glass nodule progression after dominant lesion resection. General thoracic and cardiovascular surgery, 72:183-191, 2024
4. Suzuki J, Miyoshi T, Tane K, Onodera K, Koike Y, Sakai T, Samejima J, Aokage K, Tsuboi M. The significance of regular chest computed tomography in postoperative surveillance for surgically resected non-small cell lung cancer based on TNM 8th staging system. General thoracic and cardiovascular surgery, 72:346-354, 2024
5. Niimi T, Samejima J, Wakabayashi M, Miyoshi T, Tane K, Aokage K, Taki T, Nakai T, Ishii G, Kikuchi A, Yoshioka E, Yokose T, Ito H, Tsuboi M. Ten-year follow-up outcomes of limited resection trial for radiologically less-invasive lung cancer. Japanese journal of clinical oncology, 54:479-488, 2024
6. Nomura K, Aokage K, Kaminuma Y, Nakai T, Wakabayashi M, Ikeno T, Koike Y, Taki T, Miyoshi T, Tane K, Samejima J, Ishii G, Tsuboi M. EGFR mutation impacts recurrence in high-risk early-stage lung adenocarcinoma in the IASLC grading system. International journal of clinical oncology, 29:248-257, 2024
7. Koike Y, Aokage K, Wakabayashi M, Ikeno T, Onodera K, Samejima J, Miyoshi T, Tane K, Suzuki K, Tsuboi M. Long-term outcomes of 5-year survivors without recurrence after the complete resection of non-small cell lung cancer after lobectomy: a landmark analysis in consideration of competing risks. Surgery today, 54:1005-1014, 2024
8. Nagasaki Y, Taki T, Nomura K, Tane K, Miyoshi T, Samejima J, Aokage K, Ohtani-Kim SJ, Kojima M, Sakashita S, Sakamoto N, Ishikawa S, Suzuki K, Tsuboi M, Ishii G. Spatial intratumor heterogeneity of programmed death-ligand 1 expression predicts poor prognosis in resected non-small cell lung cancer. Journal of the National Cancer Institute, 116:1158-1168, 2024
9. Goto E, Taki T, Nomura K, Miyakami Y, Miyoshi T, Tane K, Samejima J, Aokage K, Nagamine M, Sakashita S, Sakamoto N, Kojima M, Suzuki K, Tsuboi M, Ishii G. Clinicopathological differences between EGFR mutated and EGFR wild-type lung adenocarcinoma with papillary predominant pattern. Lung cancer (Amsterdam, Netherlands), 192:107830, 2024
10. Ohtani-Kim SJ, Samejima J, Wakabayashi M, Tada M, Koike Y, Miyoshi T, Tane K, Aokage K, Tsuboi M. Effect of Resected Lung Volume on Pulmonary Function and Residual Lung Volume in Patients Undergoing Segmentectomy: A Retrospective Study. Annals of surgical oncology, 31:6645-6651, 2024
11. Koike Y, Aokage K, Osame K, Wakabayashi M, Miyoshi T, Suzuki K, Tsuboi M. Risk Factors of Severe Postoperative Complication in Lung Cancer Patients with Diabetes Mellitus. Annals of thoracic and cardiovascular surgery, 30:24-00018, 2024
12. Ohtani-Kim SJ, Samejima J, Wakabayashi M, Tada M, Koike Y, Miyoshi T, Tane K, Aokage K, Tsuboi M. What is the Optimal Resection Extent for Preserving Respiratory Function in Segmentectomy?: Insights on Lung Resection Volume and Respiratory Function. Annals of surgical oncology, 31:5766-5767, 2024
13. Niimi T, Samejima J, Koike Y, Miyoshi T, Tane K, Aokage K, Taki T, Ishii G, Tsuboi M. A case of lung metastasis from gastric cancer presenting as ground-glass opacity dominant nodules. Journal of cardiothoracic surgery, 19:365, 2024
14. Miyoshi T, Aokage K, Watanabe SI, Ito H, Sakakura N, Mun M, Yamashita M, Ohde Y, Aoki T, Nishio W, Taguri M, Tsuboi M. The effect of epidermal growth factor receptor mutation on adjuvant chemotherapy with tegafur/uracil for patients with completely resected, non-lymph node metastatic non-small cell lung cancer (> 2 cm): a multicenter, retrospective, observational study as exploratory analysis of the CSPOR-LC03 study. Japanese journal of clinical oncology, 54:1185-1193, 2024
15. Aokage K, Koyama S, Kumagai S, Nomura K, Shimada Y, Yoh K, Wakabayashi M, Fukutani M, Furuya H, Miyoshi T, Tane K, Samejima J, Taki T, Hayashi T, Matsubayashi J, Ishii G, Nishikawa H, Ikeda N, Tsuboi M. Efficacy, Safety, and Influence on the Tumor Microenvironment of Neoadjuvant Pembrolizumab plus Ramucirumab for PD-L1-Positive NSCLC: A Phase II Trial (EAST ENERGY). Clinical cancer research, 30:5584-5592, 2024
