Annual Report 2024
Department of Gastric Surgery
Takahiro Kinoshita, Masahiro Yura, Mitsumasa Yoshida, Takumi Habu, Hiromi Nagata, Masaru Komatsu, Junichiro Sano, Daiki Terajima, Ayumi Umemiya, Erika Yamada
Introduction
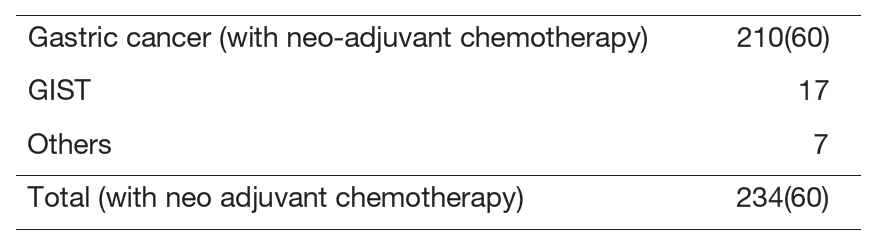
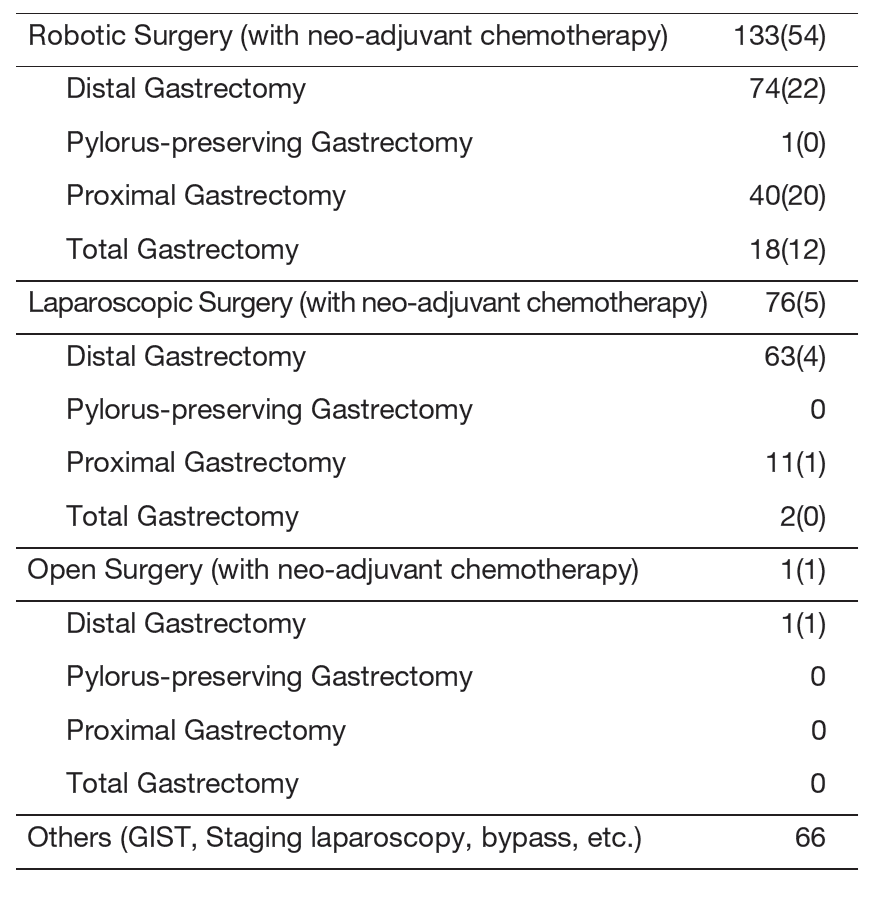
Our department consists of three staff surgeons and four junior surgeons. Our managing of tumors includes common gastric adenocarcinoma, adenocarcinoma of the esophagogastric junction (AEG: Siewert type 2/3), and gastric submucosal tumors (GIST, etc.). In 2024, we performed gastrectomy on 234 patients, either by using robotic surgery, laparoscopic or open surgery (Table 1). Laparoscopic gastrectomy was introduced in 2010, while robot-assisted gastrectomy was implemented in 2014. This year, 99% of gastrectomy was performed under laparoscopy (36%) or was robot-assisted (63%) (Table 2). The basis of our surgery is radical extirpation of cancer lesions with nodal dissection, but at the same time, organ functions and better quality of life (QOL) should be maintained. In addition, we strive to obtain better clinical outcomes for patients with diseases with dismal prognoses (type 4 gastric cancer or with progressive metastasis) through surgery combined with a modern perioperative chemotherapy in cooperation with medical oncologists.
The Team and What We Do
Usually, 10-14 patients are hospitalized and five to seven patients undergo operations per week. Our department conducts clinical conferences weekly to decide on our treatment strategies. Further, a conference with internal medicine is held weekly including doctors from Medical Oncology and Gastrointestinal Endoscopy, to discuss accurate diagnosis of the patients to decide the optimal treatment method. Robot/laparoscopic surgery covers distal, proximal, pylorus-preserving, and total gastrectomy. D2 dissection can also be performed, with indication extending to locally advanced cancer or cancer after NAC. Recently, due to the progress of chemotherapy regimen, down-staging from cStageIV is sometimes seen. For such patients, we selectively perform conversion surgery to achieve favorable outcomes. For AEGs, the transhiatal approach, thoraco-laparoscopic Ivor-Lewis surgery or mediastinoscopy-assisted esophagectomy can be performed mostly by robotic approach.
Research Activities
We aggressively publish our clinical research data at domestic or international congresses. In addition, we participate in multi-institutional clinical trials conducted by the Japan Clinical Oncology Group (JCOG) – Gastric Surgery Study Group or other international and domestic organizations, and work as PI for some clinical trials (JCOG1809) (COSMOS-GC, MONSTAR-3 regarding liquid biopsy). We have started investigating the auto intelligence technology relevant to laparoscopic or robot-assisted surgery.
Clinical Trials
The ongoing list of multi-institutional clinical trials we participate in is shown below.
1) JCOG1809 Single-arm phase II trial to evaluate safety of Laparoscopic Total Gastrectomy with Spleen-PReservING splenic hilar dissection for proximal gastric cancer invading the greater curvature (LTG-SPRING-PII)
2) JCOG1509 Phase III trial to evaluate the efficacy of neoadjuvant chemotherapy with S-1 plus oxaliplatin followed by D2 gastrectomy with adjuvant S-1 in locally advanced gastric cancer (NAGISA trial)
3) JCOG1711 Randomised controlled phase III trial to evaluate Omentum preserving gastrectomy for patients with ADvanced Gastric Cancer (ROAD-GC)
4) JCOG1907 Randomized controlled phase III trial to investigate superiority of robot-assisted gastrectomy over laparoscopic gastrectomy for clinical stage T1-2N0-2 Gastric Cancer patients (MONA-LISA Study)
5) JCOG2204 A randomized phase II study to compare the pathological responses of neoadjuvant chemotherapy for type 4 or large type 3 gastric cancer: 5-FU, Oxaliplatin and Docetaxel (FLOT) versus Docetaxel, Oxaliplatin and S-1(DOS)
6) An open label phase 2 study to evaluate the safety and efficacy of lenvatinib with pembrolizumab in the neoadjuvant / adjuvant treatment for patients with gastric cancer (EPOC2001)
7) An open label phase 2 study to evaluate the efficacy and safety of trastuzumab deruxtecan (T-DXd) in the neoadjuvant treatment for patients with HER2 positive gastric and gastroesophageal junction adenocarcinoma (EPOC2003)
8) Multiomics data cancer diagnostics therapies (TITANIA Study)
9) Conquer Solid Malignancies by blood screening –gastric cancer- 01 (COSMOS-GC)
10) Development of a Clinical Decision Support System (CDSS) with Artificial Intelligence for Gastric and Esophageal Adenocarcinomas (Ask Bob Study)
11) The HOLD Study– StomacH Cancer Elective Surgery MOrbidity and Mortality at 90-Day / The OUTLIVE Study - Oesophageal and JUncTional Cancer ELectIVE Surgery Morbidity and Mortality at 90-Day: A TUGS Multinational Audit
12) The UGIRA International Registry for Robot-Assisted Minimally Invasive Gastrectomy (RAMIG) for gastric cancer
13) The UGIRA International Registry for Robot-Assisted Minimally Invasive Esophagectomy (RAMIE)
14) A Study on the Learning Curve of the Multi-Jointed Articulating Laparoscopic Instrument (ArtiSential)
15) Phase-II Study to Evaluate the Efficacy and Safety of Total Neoadjuvant Therapy (TNT) Including Pembrolizumab + FLOT + Short-Term Radiation Therapy for Resectable EGJ Adenocarcinoma (EPOC2301)
Education
Resident doctors are trained to become specialized surgical oncologists with sufficient techniques and knowledge. Nowadays, these doctors are given opportunities to perform the minimally invasive surgeries (robotic/laparoscopic). In 2024, three doctors from our department have been certified as the skill-qualified surgeon of the Japan Society for Endoscopic Surgery. We also place importance on the education of surgeons from other institutions. A total of 20 doctors from 9 countries visited us and stayed for several months for surgery observations, and one Colombian doctor took the advanced clinical training program in our department which was officially approved by the Japanese government.
List of papers published in 2024
Journal
1. Kooij CD, de Jongh C, Kingma BF, van Berge Henegouwen MI, Gisbertz SS, Chao YK, Chiu PW, Rouanet P, Mourregot A, Immanuel A, Mala T, van Boxel GI, Carter NC, Li H, Fuchs HF, Bruns CJ, Giacopuzzi S, Kalff JC, Hölzen JP, Juratli MA, Benedix F, Lorenz E, Egberts JH, Haveman JW, van Etten B, Müller BP, Grimminger PP, Berlth F, Piessen G, van den Berg JW, Milone M, Luketich JD, Sarkaria IS, Sallum RAA, van Det MJ, Kouwenhoven EA, Brüwer M, Harustiak T, Kinoshita T, Fujita T, Daiko H, Li Z, Ruurda JP, van Hillegersberg R. The Current State of Robot-Assisted Minimally Invasive Esophagectomy (RAMIE): Outcomes from the Upper GI International Robotic Association (UGIRA) Esophageal Registry. Annals of surgical oncology, 32:823-833, 2025
2. Tomi Y, Kinoshita T, Yura M, Sakamoto N, Fujita T, Tokunaga M, Kinugasa Y. Accuracy of the preoperative estimation of esophageal invasion length of adenocarcinoma of the esophagogastric junction and its discrepancy with the pathological measurement. Surgery today, 55:768-777, 2025
3. Nagata H, Kinoshita T, Sakashita S, Kojima M, Taki T, Kuwata T, Yura M, Shitara K, Ishii G, Sakamoto N. Area of Residual Tumor Measurement After Preoperative Chemotherapy as an Objective and Quantitative Method for Predicting the Prognosis of Gastric Cancer: A Single-Center Retrospective Study. World journal of surgery, 49:717-726, 2025
4. Amini N, Kinoshita T, Arrieta M, Yoshida M, Nagata H, Habu T, Komatsu M, Yura M. Novel Robotic Valvuloplastic Esophagogastrostomy Technique After Proximal Gastrectomy: A Safety and Feasibility Study. Surgical laparoscopy, endoscopy & percutaneous techniques, 35:e1322, 2025
5. Harada K, Sakamoto N, Kitaoka T, Nakamura Y, Kondo R, Morisue R, Hashimoto H, Yamamoto Y, Ukai S, Maruyama R, Sakashita S, Kojima M, Tanabe K, Ohdan H, Shitara K, Kinoshita T, Ishii G, Yasui W, Ochiai A, Ishikawa S. PI3 expression predicts recurrence after chemotherapy with DNA-damaging drugs in gastric cancer. The Journal of pathology, 265:472-485, 2025
6. Akimoto E, Kinoshita T, Yura M, Yoshida M, Okayama T, Habu T, Komatsu M, Nagata H, Terajima D. Feasibility of laparoscopic/robot-assisted surgery for Borrmann type 4 gastric cancer: a comparison study with conventional open surgery. Surgical endoscopy, 38:3337-3345, 2024
7. Habu T, Kumagai S, Bando H, Fujisawa T, Mishima S, Kotani D, Nakamura M, Hojo H, Sakashita S, Kinoshita T, Yano T, Mitsunaga S, Nishikawa H, Koyama S, Kojima T. Definitive chemoradiotherapy induces T-cell-inflamed tumor microenvironment in unresectable locally advanced esophageal squamous cell carcinoma. Journal of gastroenterology, 59:798-811, 2024
8. Yoshida M, Kitaguchi D, Takeshita N, Matsuzaki H, Ishikawa Y, Yura M, Akimoto T, Kinoshita T, Ito M. Surgical step recognition in laparoscopic distal gastrectomy using artificial intelligence: a proof-of-concept study. Langenbeck's archives of surgery, 409:213, 2024
9. Kitaoka T, Harada K, Sakashita S, Kojima M, Taki T, Kuwata T, Kinoshita T, Futakuchi M, Ishii G, Sakamoto N. Quantification of Gremlin 1 throughout the tumor stroma using whole slide imaging and its clinicopathological significance in gastric cancer. Virchows Archiv, 485:1107-1116, 2024
10. Uyama I, Shibasaki S, Inaki N, Ehara K, Oshiro T, Okabe H, Obama K, Kasama K, Kinoshita T, Kurokawa Y, Kojima K, Shiraishi N, Suda K, Takiguchi S, Tokunaga M, Naitoh T, Nagai E, Nishizaki M, Nunobe S, Fukunaga T, Hosoda K, Sano T, Sagawa H, Shindo K, Nakagawa M, Hiratsuka T. Practice guidelines on endoscopic surgery for qualified surgeons by the endoscopic surgical skill qualification system: Stomach. Asian journal of endoscopic surgery, 17:e13365, 2024
11. Manuel AG, Kinoshita T, Amini N, Akimoto E, Yura M, Yoshida M, Habu T, Nagata H, Komatsu M, Sano J, Terajima D. Oncological long-term outcomes of laparoscopic versus open gastrectomy for cT3-4 gastric cancer at surgical staging: a propensity-score matched cohort study. Surgical endoscopy, 38:6682-6690, 2024
12. Nagata H, Kinoshita T, Komatsu M, Habu T, Yoshida M, Yura M. Comparison of robotic versus laparoscopic total gastrectomy for gastric cancer: A single-center retrospective cohort study in a Japanese high-volume center. European journal of surgical oncology, 50:108706, 2024
13. Minakata N, Kadota T, Sakashita S, Inaba A, Sunakawa H, Takashima K, Nakajo K, Murano T, Shinmura K, Yoda Y, Ikematsu H, Fujita T, Kinoshita T, Yano T. Tumor thickness is associated with metastasis in patients with submucosal invasive adenocarcinoma of the esophagogastric junction. Diseases of the esophagus, 37:doae083, 2024
14. Yamada Y, Nagashima K, Azuma M, Masutani M, Ichikawa H, Iwasa S, Takahashi N, Hirano H, Kanato K, Machida N, Kinoshita T, Hata H, Kawakami H, Takahari D, Boku N, Kurokawa Y, Terashima M, Yoshikawa T, Sekine S, Hiraoka N. Predictive and prognostic value of excision repair cross-complementing group 1 in patients with advanced gastric cancer. BJC reports, 2:18, 2024
15. Okano W, Matsuura K, Hayashi R, Tomioka T, Shinozaki T. Management of Treatment for laryngeal and Hypopharyngeal Cancer Surgery Patients Using Geriatric Assessment. Koutou (THE LARYNX JAPAN), 36:84-87, 2024
16. Takei S, Kawazoe A, Jubashi A, Komatsu M, Sato K, Mishima S, Kotani D, Yura M, Sakamoto N, Sakashita S, Kuwata T, Kojima T, Fujita T, Kinoshita T, Shitara K. Safety and efficacy of perioperative FLOT regimen in Japanese patients with gastric, esophagogastric junction, or esophageal adenocarcinoma: A single-institution experience. ESMO Gastrointestinal Oncology, 4:100050, 2024
