Annual Report 2024
Department of Palliative Medicine
Tomofumi Miura, Emi Kubo, Mitsue Takeuchi, Yukako Hattori, Yuya Ashitomi, Koshin Katsu, Mariko Harada, Sakiho Noda, Tamao Yoshida, Shoko Aoki, Rumiko Osawa, Chiharu Higashiono
Introduction
The purpose of our department is to improve the quality of life of cancer patients and their family caregivers by managing the irritable symptom burden and establishing a regional palliative care system. To achieve this goal, we provide 3 palliative care services: (1) outpatient clinic, (2) palliative care unit, and (3) supportive care team. Since 2018, the National Cancer Center Hospital East has been recognized as an ESMO Designated Centre of Integrated Oncology and Palliative Care.
The Team and What We Do
1. Outpatient clinic
Patients with or without anti-cancer therapy consult our outpatient clinic about management of their symptoms or support to decide where and how to spend their lives (Table 1).
Table 1. Number of patients in the outpatient clinic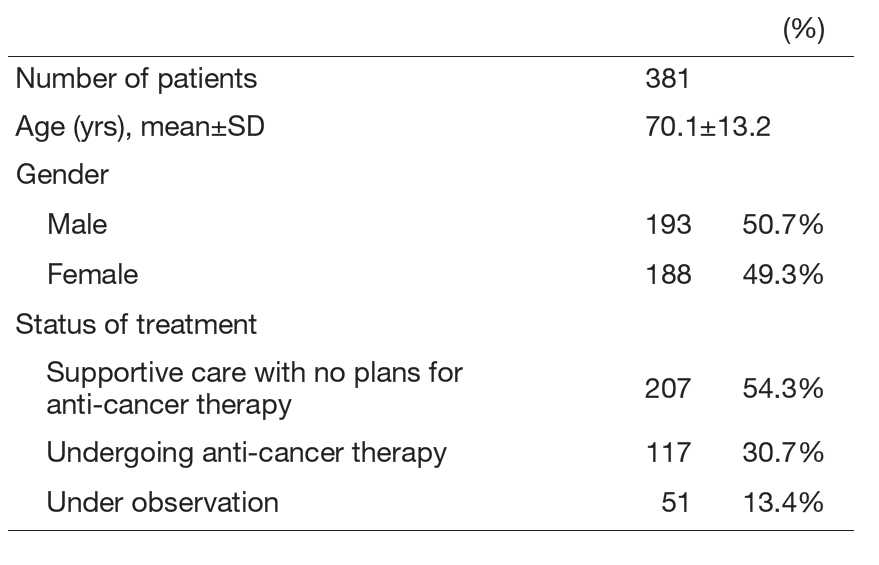

2. Palliative care unit
Our palliative care unit is the Japanese version of an acute palliative care unit (APCU). The features of APCUs are multidimensional assessment, rapid symptom control, and intensive psychosocial care with a shorter length of stay and lower death rate than in a traditional PCU. Medical social workers greatly contribute to the transition to palliative home care and transfers to other hospitals (Table 2).
Table 2. Number of patients in the PCU 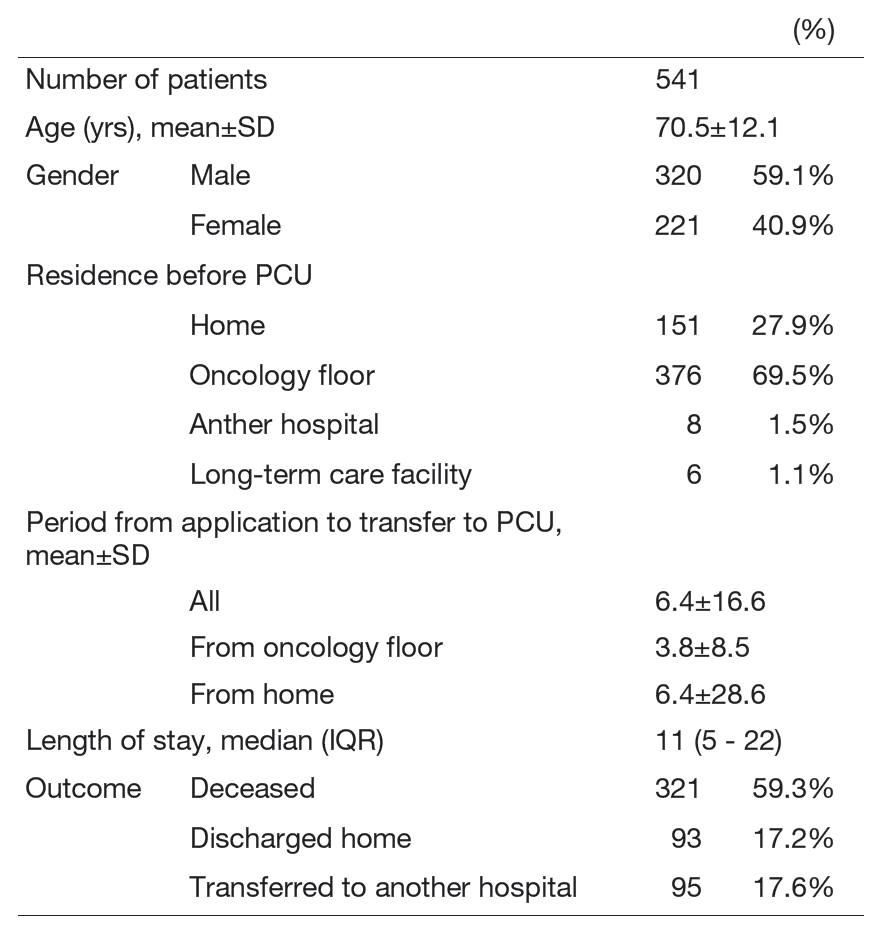

3. Supportive care team
This team consists of physicians, psycho-oncologists, nurses, dieticians, physiotherapists, and speech-language-hearing therapists. In the oncology section, our supportive care team takes a multidisciplinary approach for inpatients with various illnesses (Table 3).
Table 3. Number of patients treated by the supportive care team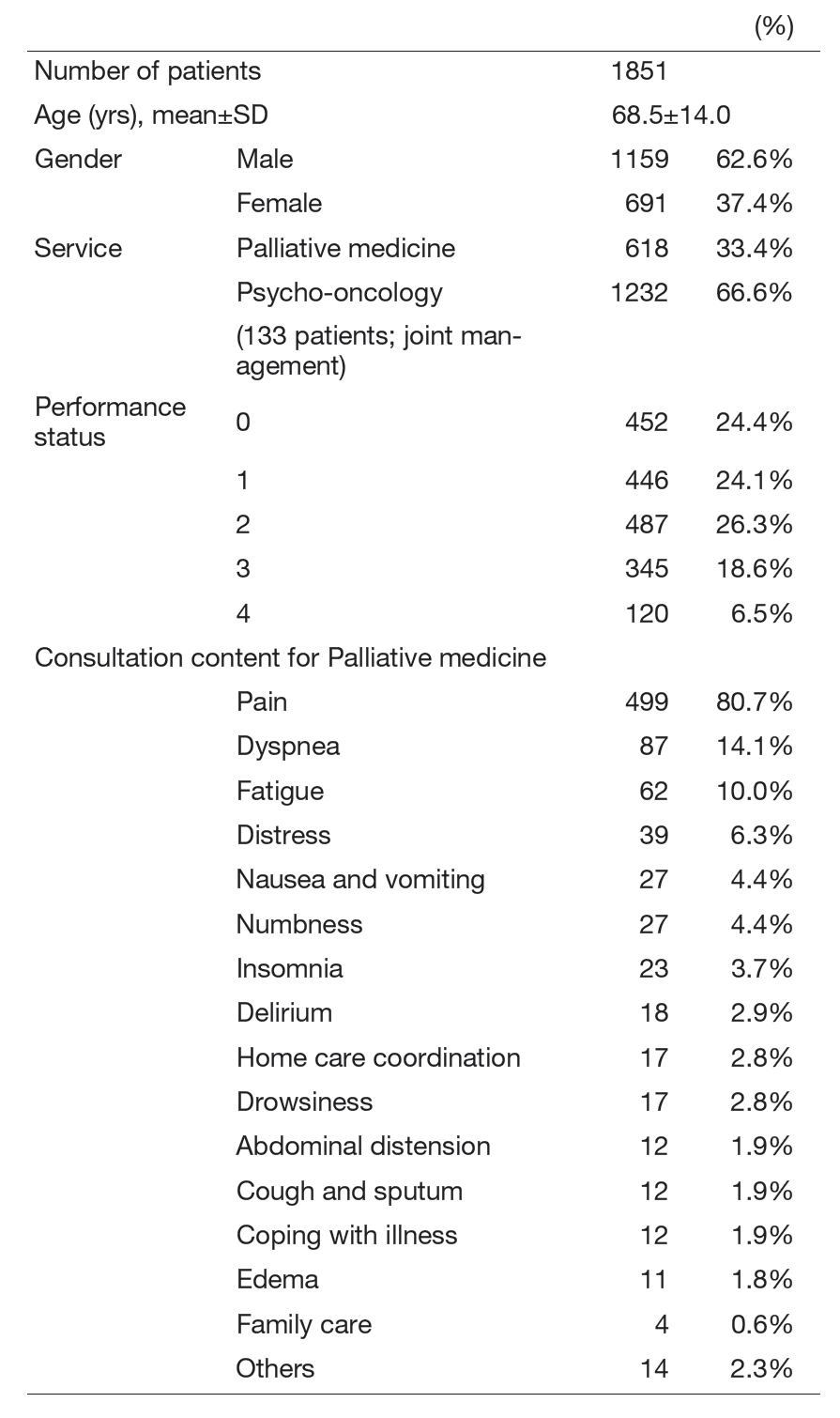

Research Activities
1) Investigator-initiated clinical trial of alternating magnetic field therapy for chemotherapy-induced peripheral neuropathy (CIPN)
2) Development of a symptom monitoring system using voice-based interaction
3) Development of an online peer-support program for patients
4) Prospective observational study of patient support through social network services (SNS nursing)
5) Development of a non-contact vital-sign monitoring device
6) Exploratory randomized controlled trial of healing effects using inaudible sound frequencies
7) Clinical trial of alternating magnetic field therapy for cancer-related pain
8) Development of a smart consultation room that transmits patients’ stress status to healthcare providers in a non-contact manner
9) Development of a digital Comprehensive Geriatric Assessment (CGA) system for older patients using non-contact technology
10) Participation in multicenter observational studies, interventional studies, and surveys of bereaved families.
Clinical Trials
1) A double-blind randomized controlled trial to relief the distress from chemotherapy-induced peripheral neuropathy using magnetic fields
2) Prospective observational study to evaluate the psychosocial effects of participation in an online peer-support group among rare cancer patients with dependent children
3) Exploratory randomized controlled study on the impact of high-resolution natural sounds beyond the audible range on biometrics and healing in patients with advanced cancer
Education
The purpose of our training program is to promote medical residents’ understanding of palliative care for cancer patients and their families. Residents may also receive training in home-based palliative care upon request.
Future Prospects
Our department will continue these activities and pursue the development of novel treatments and medical devices to further improve the quality of life of cancer patients and their family caregivers.
List of papers published in 2024
Journal
1. Hasuo H, Ishiki H, Matsuda Y, Matsuoka H, Kosugi K, Xing M, Akiyama Y, Matsumoto Y, Ishikawa H. Trigger point injections for myofascial pain in terminal cancer: a randomized trial. Pain medicine (Malden, Mass.), 26:14-21, 2025
2. Gotoh R, Shimizu Y, Hayashi A, Isseki M, Miura T, Inoue A, Takano M, Masukawa K, Aoyama M, Morita T, Kizawa Y, Tsuneto S, Shima Y, Miyashita M. Associations Between Anticipatory Grief and Post-Bereavement Depression and Post-Loss Grief of Family Members of Dying Patients With Cancer in Palliative Care Units: A Cohort Study. The American journal of hospice & palliative care, 10499091241313299, 2025
3. Amano K, Okamura S, Miura T, Baracos VE, Mori N, Sakaguchi T, Uneno Y, Ishiki H, Hiratsuka Y, Yokomichi N, Hamano J, Baba M, Mori M, Morita T. Clinical Implications of the C-Reactive Protein-Albumin Ratio as a Prognostic Marker in Terminally Ill Patients with Cancer. Journal of palliative medicine, 28:592-600, 2025
4. Shimotsuura Y, Ishizuka K, Kawaguchi T, Umetsu K, Harada M, Inoue Y, Kubo E, Kosugi K, Igarashi T, Enomoto S, Taniyama H, Iwata T, Yamaguchi T, Matsumoto Y, Miura T. Effects of High-Resolution Natural Sound with Inaudible High-Frequency Components on Healing, Symptoms, and Sleep Satisfaction in Terminally Ill Cancer Patients. Palliative medicine reports, 6:53-60, 2025
5. Noda S, Yamaguchi J, Kosugi K, Ishida A, Harada M, Ishizuka K, Inoue Y, Kubo E, Miura T. Peppermint Inhalation Therapy for Persistent Hiccups in Terminally Ill Cancer Patient: A Case Study. Journal of pain and symptom management, 67:e503-e505, 2024
6. Amano K, Okamura S, Baracos V, Mori N, Sakaguchi T, Uneno Y, Hiratsuka Y, Hamano J, Miura T, Ishiki H, Yokomichi N, Hatano Y, Morita T, Mori M. Fluid retention and weight loss in refractory cancer cachexia. BMJ supportive & palliative care, spcare-2024-004820, 2024
7. Amano K, Baracos VE, Mori N, Okamura S, Yamada T, Miura T, Tatara R, Kessoku T, Matsuda Y, Tagami K, Otani H, Mori M, Taniyama T, Nakajima N, Nakanishi E, Kako J, Morita T, Miyashita M. Associations of nutrition impact symptoms with dietary intake and eating-related distress in patients with advanced cancer. Clinical nutrition ESPEN, 60:313-319, 2024
8. Amano K, Okamura S, Baracos VE, Mori N, Sakaguchi T, Uneno Y, Hiratsuka Y, Hamano J, Miura T, Ishiki H, Yokomichi N, Hatano Y, Morita T, Mori M. Impacts of fluid retention on prognostic abilities of cachexia diagnostic criteria in cancer patients with refractory cachexia. Clinical nutrition ESPEN, 60:373-381, 2024
9. Yanai M, Aoyama M, Kosugi K, Tsumura A, Nakanishi E, Miyashita M. Reliability and validity of the Japanese version of the Parenting Concerns Questionnaire. Japanese journal of clinical oncology, 54:797-804, 2024
10. Okamura N, Kubo E, Ishida A, Noda S, Harada M, Ishizuka K, Inoue Y, Kosugi K, Miura T. Differences in discharge letter content: oncologists' vs. home care physicians' needs. Supportive care in cancer, 32:299, 2024
11. Amano K, Okamura S, Matsuda Y, Baracos VE, Mori N, Miura T, Tatara R, Kessoku T, Tagami K, Otani H, Mori M, Taniyama T, Nakajima N, Nakanishi E, Kako J, Morita T, Miyashita M. Associations of nutrition impact symptoms with depression in patients with advanced cancer. Supportive care in cancer, 32:445, 2024
12. Shimizu Y, Hayashi A, Maeda I, Miura T, Inoue A, Takano M, Aoyama M, Masukawa K, Miyashita M. Resilience and coping styles in family caregivers of terminally ill patients: A cross-sectional survey. Palliative & supportive care, 23:e12, 2024
13. Matsumoto Y, Umemura S, Okizaki A, Fujisawa D, Yamaguchi T, Oyamada S, Miyaji T, Mashiko T, Kobayashi N, Satomi E, Kiuchi D, Morita T, Uchitomi Y, Goto K, Ohe Y. Nurse-Led Screening-Triggered Early Specialized Palliative Care Program for Patients With Advanced Lung Cancer: A Multicenter Randomized Controlled Trial. Cancer medicine, 13:e70325, 2024
14. Matsumoto Y, Uehara Y, Mizushima A, Kosugi T, Sone M, Nakamura N, Miyashita M, Morita T, Yamaguchi T, Satomi E. Availability of, Barriers to Performing, and Educational Practices of Interventional Procedures for Refractory Pain in Cancer Patients: A Nationwide Survey of Designated Cancer Hospitals in Japan. Palliative medicine reports, 5:543-552, 2024
