Annual Report 2024
Department of Esophageal Surgery
Staff : Hiroyuki Daiko, Koshiro Ishiyama, Daisuke Kurita, Yasuyuki Seto
Resident : Daichi Utsunomiya, Eigo Akimoto, Shota Igaue, Ryoko Nozaki, Ryuta Kakuta
Introduction
The Department of Esophageal Surgery deals with neoplasms arising from the esophagus. The surgical management of esophageal cancer has been the main clinical research activity of this department. In particular, our department is striving to establish multimodal surgical treatment that consists of neoadjuvant treatment followed by minimally invasive esophagectomy. Our department is conducting a study to define the role of robotic surgery in the multimodal approach to the treatment of esophageal cancer. Robotic esophagectomy with gastric reconstruction has already been established as a standard approach in our department, and a feasibility study of SP robotic esophagectomy via subcoastal is now underway.
The Team and What We Do
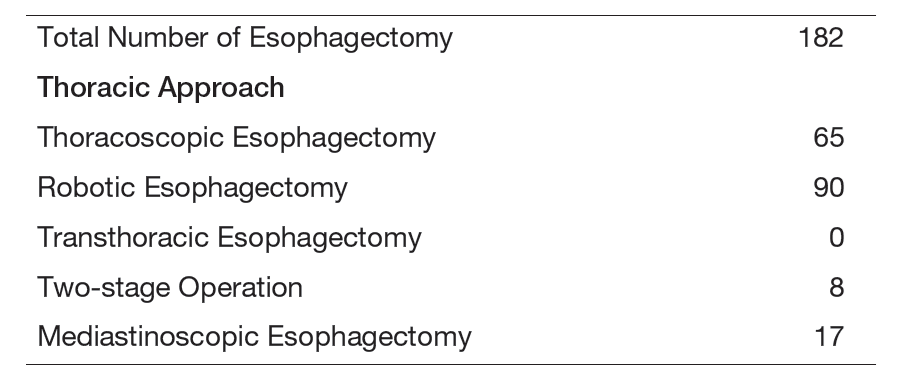
The Department of Esophageal Surgery consists of three staff surgeons and five residents. An Esophageal Conference is held every Wednesday evening to discuss the diagnosis, staging, and treatment strategy for each patient and is attended by surgeons, medical oncologists, endoscopists, radiologists, radiation oncologists, and head & neck surgeons. Approximately four patients undergo surgery every week. In 2024, 182 patients underwent esophagectomies. Thoracoscopic and robotic esophagectomy with extended lymph node dissection were performed on 65 and 90 cases, respectively. Bilateral transcervical mediastinoscopic laparoscopic-assisted esophagectomy for patients over 80 years of age or patients with multiple complications was performed in 17 cases. Postoperatively, within 30 days, no patients died after esophagectomy.
Research Activities
Currently, our department is examining the role of robotic surgery as a minimally invasive esophagectomy that consists of robotic esophagectomy and robotic reconstruction. Even for patients with radical chemoradiotherapy and conversion chemotherapy for cT4b, robotic esophagectomy and robotic gastric reconstruction have already become a standard surgical procedure for esophageal cancer.
For treating patients aged over 80 years or at high risk, a two-stage surgical procedure divided into resection and reconstruction is being attempted.
Bilateral transcervical esophagectomy has been developed in our institution. We are evaluating the efficacy of the novel ultimate surgical approach of bilateral transcervical esophagectomy.
The feasibility studies of HINOTORI for esophageal carcinoma and SP esophagectomy via subcoastal are ongoing.
Our department is also studying the role and efficacy of conversion surgery for cT4b in the multimodal treatment of esophageal cancer.

Clinical Study
1. A clinical study on short-term outcomes of robotic-assisted esophagectomy and robotic-assisted gastric reconstruction for esophageal cancer (excluding T4 cases with bone invasion or lymph node metastasis) using the hinotoriTM Surgical Robot System
2. Prospective observational study aimed at developing a method to predict the efficacy of preoperative chemotherapy for esophageal cancer using genomic profiling and ctDNA measurement
3. A single-arm phase II clinical trial investigating the effects of synbiotics on perioperative management for resectable esophageal cancer
4. A study on the clinical usefulness of a newly developed fermented lactic acid-based liquid diet for postoperative early enteral nutrition in patients with malignant esophageal tumors
5. A study on multi-organ segmentation AI using CT images of patients with esophageal cancer
6. A study on 3D computer graphic reconstruction of organs from CT/MRI images of patients with esophageal cancer
7. A study on brainwave activity of surgeons during robotic-assisted surgery
List of papers published in 2024
Journal
1. Fujita T, Shigeno T, Kajiyama D, Sato K, Fujiwara N, Daiko H. A novel device to assess the oxygen saturation and congestion status of the gastric conduit in thoracic esophagectomy. BMC Surg24:17, 2024.
2. Kato T, Tsukamoto S, Miyake M, Kudose Y, Takamizawa Y, Moritani K, Daiko H, Kanemitsu Y. Prognostic impact of extramural venous invasion detected by contrast-enhanced CT colonography in colon cancer. BJS Open8: zrad 121, 2024.
3. Fukushima T, Watanabe N, Okita Y, Yokota S, Kurita D, Ishiyama K, Oguma J, Kawai A, Daiko H. Preoperative physical activity is associated with prognosis in patients with esophageal cancer undergoing thoracoscopic-laparoscopic esophagectomy after neoadjuvant chemotherapy. Gen Thorac Cardiovasc Surg 72:134-143, 2024.
4. Fujita T, Sato K, Fujiwara N, Kajiyama D, Shigeno T, Daiko H. A novel imaging technology to assess tissue oxygen saturation and its correlation with indocyanine green in the gastric conduit during thoracic esophagectomy. Surgery 175:360-367, 2024.
5. Igaue S, Nozaki R, Utsunomiya D, Kubo Y, Kubo K, Kurita D, Yamamoto S, Ishiyama K, Oguma J, Daiko H.Significance of Surgery for Resectable M1 Lymph Node Metastases Without Organ Metastasis in esophageal Carcinoma in the Era of Neoadjuvant Treatment. Ann Surg 31:1525-1535, 2024.
6. Fujita T, Sato K, Fujiwara N, Kajiyama D, Shigeno T, Otomo M, Daiko H.Robot-assisted transcervical esophagectomy with a bilateral cervical approach for thoracic esophagectomy. Surg Endosc 38:1617-1625, 2024.
7. Kubo Y, Igaue S, Utsunomiya D, Kubo K, Kurita D, Ishiyama K, Oguma J, Daiko H. Association between preoperative serum zinc level and prognosis in patients with advanced esophageal cancer in the neoadjuvant treatment era. Ann Gastroenterol Surg 8;595-603, 2024.
8. Cho H, Abe S, Nonaka S, Suzuki H, Yoshinaga S, Okuma K, Yamamoto S, Daiko H, Kato K, Sekine S, Boke N, Saito Y. Long-term outcomes after non-curative endoscopic resection for esophageal squamous cell carcinoma followed by additional chemoradiotherapy. Dis Esophagus 37;doae004, 2024.
9. Hirano Y, Konishi T, Kaneko H, Itoh H, Matsuda S, Kawakubo H, Uda K, Matsui H, Fushimi K, Daiko H, Itano O, Yasunaga H, Kitagawa Y. Antimicrobial prophylaxis with ampicillin-sulbactam compared with cefazolin for esophagectomy: Nationwide inpatient database study in Japan. Ann Surg 279:640-647, 2024.
10. Zhu Y, Xu S, Teng X, Zhao R, Peng L, Fang Q, Xiao W, Jiang Z, Li Y, Luo X, Han Y, Daiko H, Leng X. Refining postoperative monitoring of recurrent laryngeal nerve injury in esophagectomy patients through transcutaneous laryngeal ultrasonography. Esophagus 21:141-149, 2024.
11. Furuse K, Nara M, Kageyama D, Akazawa S, Daiko H, Higashino T. Pectoralis Major Muscle Flap Utilization in Salvage Esophagectomy including Great Vessel Resection Reconstructed by Prosthetic Grafts. Ann Plast Surg 92:401-404, 2024.
12. Daiko H, Ishiyama K, Kurita D, Kubo K, Kubo Y, Utsunomiya D, Igaue S, Nozaki R, Akimoto E, Kakuta R, Horonushi S, Fujita T, Oguma J. Bilateral transcervical mediastinoscopic-assisted transhiatal laparoscopic esophagectomy compared with thoracolaparoscopic esophagectomy for esophageal cancer: a propensity score-matched analysis. Surg Endosc 38:5746-5755, 2024.
13. Daiko H, Oguma J, Ishiyama K, Kurita D, Kubo K, Kubo Y, Utsunomiya D, Igaue S, Nozaki R, Leng X, Fujita T, Fujiwara H. Technical feasibility and oncological outcomes of robotic esophagectomy compared with conventional thoracoscopic esophagectomy for clinical T3 or T4 locally advanced esophageal cancer: a propensity-matched analysis. Surg Endosc 38:3590-3601,2024.
14. Kato K, Machida R, Ito Y, Daiko H, Ozawa S, Ogata T, Hara H, Kojima T, Abe T, Bamba T, Watanabe M, Kawakubo H, Shibuya Y, Tsubosa Y, Takegawa N, Kajiwara T, Baba H, Ueno M, Takeuchi H, Nakamura K, S, Kitagawa Y; JCOG1109 investigators. Double chemotherapy, triplet chemotherapy, or doublet chemotherapy combined with radiotherapy as neoadjuvant treatment for locally advanced oesophageal cancer (JCOG1109 NExT): a randomised, controlled, open-label, phase 3 trial. Lancet 404:55-66, 2024.
15. Hirose T, Yamamoto S, Honma Y, Yokoyama K, Hirano H, Okita N, Shoji H, Iwasa S, Takashima A, Ishiyama K, Oguma J, Daiko H, Maeda S, Kato K. Preoperative docetaxel, cisplatin, and 5-fluorouracil for resectable locally advanced esophageal and esophagogastric junctional adenocarcinoma. Esophagus 21:328-335, 2024.
16. Inoue M, Kanemitsu Y, Tsukamoto S, Moritani K, Takamizawa Y, Daiko H. Prognostic impact of primary tumour location after curative resection in Stage I-III colorectal cancer: a single-centre retrospective study. Jpn J Clin Oncol 54:753-760, 2024.
17. Kubo Y, Nozaki R, Igaue S, Utsunomiya D, Kubo K, Yamamoto S, Kurita D, Kashihara T, Ishiyama K, Honma Y, Oguma J, Kato K, Daiko H.Neoadjuvant Chemotherapy Improves Feasibility of Larynx preservation and prognosis in resectable locally advanced cervical esophageal cancer. Ann Surg Oncol 31:5083-5091, 2024.
18. Kubo Y, Kato K, Daiko H. ASO Author Reflections: Neoadjuvant Chemotherapy versus Definitive Chemoradiation Therapy for Locally Advanced Cervical Esophageal Cancer: A Retrospective Study. Ann Surg Oncol 31:5308-5309, 2024.
19. Murashima Y, Yamamoto S, Hirose T, Kadono T, Ikeda G, Ohara A, Itoyama M, Yokoyama K, Honma Y, Ishiyama K, Oguma J, Daiko H, Kato K. Efficacy and Safety of Salvage-line Nivolumab Monotherapy for Advanced Esophageal Squamous Cell Carcinoma: Comparison of 240 mg Versus 480 mg Doses. J Gastrointest Cancer 55:1345-1351, 2024.
20. Sato K, Fujita T, Otomo M, Shigeno T, Kajiyama D, Fujiwara N, Daiko H. Total RAMIE with three-field lymph node dissection by a simultaneous two-team approach using a new docking method for esophageal cancer. Surg Endosc 38:4887-4893, 2024.
21. Shigeno T, Otomo M, Kajiyama D, Sato K, Fujiwara N, Kinugasa Y, Daiko H, Fujita T. Assessing the outcomes of posterior thoracic para-aortic lymph node dissection after induction chemotherapy in patients with esophageal squamous cell carcinoma. Dis Esophagus 37:doae060, 2024.
22. Fujita T, Sato K, Fujiwara N, Kajiyama D, Kubo Y, Daiko H. Robot-assisted cervical esophagectomy with simultaneous transhiatal abdominal procedure for thoracic esophageal carcinoma. Surg Endosc 38:6413-6422, 2024.
23. Furube T, Takeuchi M, Kawakubo H, Noma K, Maeda N, Daiko H, Ishiyama K, Otsuka K, Sato Y, Koyanagi K, Tajima K, Garcia RN, Maeda Y, Matsuda S, Kitagawa Y. Usefulness of an Artificial Intelligence Model in Recognizing Recurrent Laryngeal Nerves During Robot-Assisted Minimally Invasive Esophagectomy. Ann Surg Oncol 31:9344-9351, 2024.
24. Shigeno T, Kajiyama D, Sato K, Fujiwara N, Kinugasa Y, Daiko H, Fujita T. Efficiency of conversion surgery for esophageal squamous cell carcinoma with solitary abdominal para-aortic lymph node metastasis. Surg Today 54:1490-1497, 2024.
25. Kubo K, Igaue S, Utsunomiya D, Kubo Y, Kanematsu K, Kurita D, Ishiyama K, Oguma J, Goto K, Daiko H. Preoperative neutrophil-to-lymphocyte ratio predicts recurrence of esophageal squamous cell carcinoma after neoadjuvant triplet chemotherapy. Gen Thorac Cardiovasc Surg 72:802-809, 2024.
26. Yamamoto S, Kato K, Daiko H, Ito Y, Kajiwara T, Kojima T, Miyata H, Nakagawa S, Ueno M, Watanabe M, Tsunoda S, Abe T, Nagatani Y, Okada M, Morita M, Sato T, Mizusawa J, Nakamura K, Kitagawa Y. Factors influencing decision-making between surgery and chemoradiotherapy for esophageal carcinoma from the JCOG0502. Future Oncol 20:2849-2854, 2024.
27. Igaue S, Daiko H. ASO Author Reflections: Multimodal Treatment, Including Surgery, for Patients with Resectable M1 Lymph Node Metastases Without Organ Metastasis in Esophageal Carcinoma Showed Promising Prognosis. Ann Surg Oncol31:1581-1582, 2024.
