Annual Report 2024
Department of Hepatobiliary and Pancreatic Surgery
Minoru Esaki, Satoshi Nara, Akinori Miyata, Takahiro Mizui, Ryosuke Umino
Introduction
The Department of Hepatobiliary and Pancreatic Surgery provides advanced surgical care for patients with malignant tumors of the liver, biliary tract, and pancreas. Our team specializes in highly challenging cancers such as pancreatic and biliary tract malignancies, aiming to deliver treatment that balances safety with curative intent through appropriate perioperative management, advanced surgical techniques, and extensive clinical experience in cooperation with the Department of Diagnostic Radiology, the Department of Hepatobiliary and Pancreatic Oncology and the Department of Diagnostic Pathology.
The Team and What We Do
Our department consists of five staff surgeons, two cancer specialist fellows, and four to five resident physicians working together as a team. We perform more than 400 surgical procedures each year. One staff surgeon and one resident are in charge of each patient, perform the operation and provide perioperative care. The chief resident attends almost all the operations, supervises the residents and manages the care of all patients in the ward.
Conferences
Regular conferences are held to ensure comprehensive treatment planning and to share and provide feedback on surgical outcomes.
- Ward conference (three times weekly): Discussion of the clinical management of perioperative patients and surgical strategies.
- "Cherry conference" (weekly): Multidisciplinary review of imaging studies by surgeons, endoscopists, oncologists, radiologists, and sonographers.
- Hepatobiliary and pancreatic (HBP) case conference: Joint meeting of surgeons, endoscopists, and oncologists focusing on treatment strategies for new patients.
- Micro-conference (pathology): Postoperative cases are reviewed with participation from surgeons, oncologists, radiologists, endoscopists, and pathologists.
Clinical practice for HBP malignancies
The number of diseases and surgical treatments are shown in Tables 1 and 2.
Table 1. Diagnosis for surgical treatment (between April 2024 and March 2025)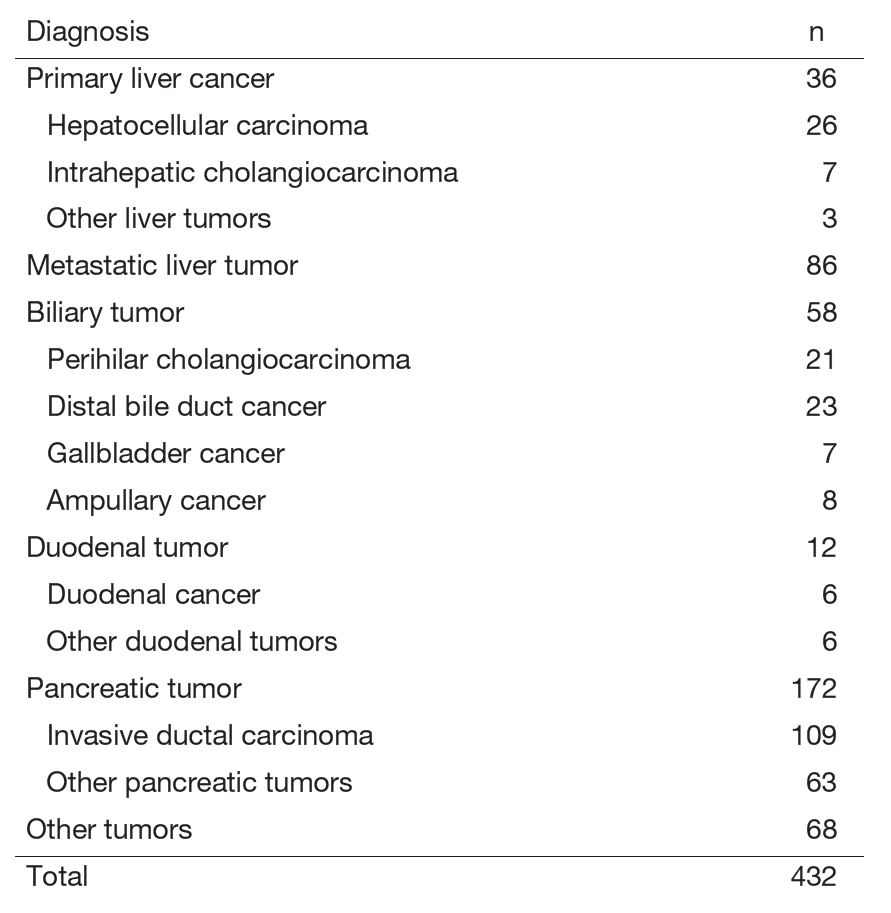

Table 2. Surgical procedures (between April 2024 and March 2025)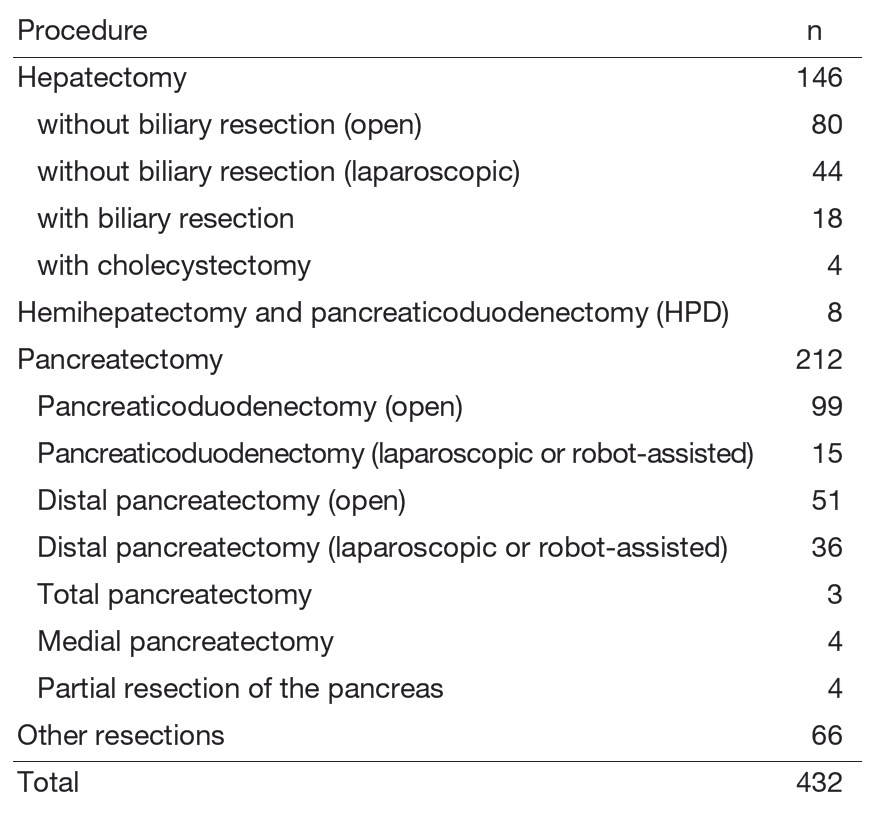

- Pancreatic cancer: Multidisciplinary treatments combining curative resection along with neoadjuvant and adjuvant chemotherapy constitute the standard strategy. Thanks to recent advances in systemic chemotherapy with improved response, opportunities for conversion surgery in initially unresectable locally advanced cases have been increasing.
- Biliary tract cancer (ampullary cancer, cholangiocarcinoma, gallbladder cancer): Based on careful imaging evaluations of tumor extension, a wide variety of surgical resections are applied, including hepatopancreatoduodenectomy with or without vascular reconstruction. Safe and curative resection with meticulous perioperative management is essential.
- Hepatocellular carcinoma: Surgical resection is usually indicated for patients with solitary or a few tumors and with favorable hepatic function. Resection is also indicated for large tumors or cases with macroscopic vasculobiliary tumor thrombosis, provided sufficient hepatic function and remnant liver volume. Alternative treatments, including radiofrequency ablation, and transarterial chemoembolization, are offered in collaboration with oncologists and radiologists.
- Minimally invasive surgery: Laparoscopic or robot-assisted hepatectomy is considered the first treatment choice for most liver tumors. Laparoscopic or robot-assisted pancreaticoduodenectomy, distal pancreatectomy and spleen-preserving distal pancreatectomy are also performed, especially for low-grade malignant pancreatic tumors. Based on our experience, the indication is gradually being extended to pancreatic head ductal adenocarcinoma.
Research Activities
We actively promote clinical research in the HBP field, aiming to establish new standards of care and improve outcomes.
Investigator-Initiated Studies
- JCOG1920: A phase III trial of neoadjuvant GCS therapy for resectable biliary tract cancer, led by our department (PI: Dr. Nara), has been underway since March 2021 and is nearing completion of patient enrollment.
- PLaG-PC-01 study: A prospective observational study investigating the clinical significance of ctDNA in peritoneal lavage samples from resectable pancreatic ductal adenocarcinoma, initiated in September 2023, has reached 75% of the planned accrual and is expected to complete within the next year.
- Multicenter study on intraoperative navigation: A collaborative study on the utility of fusion imaging–based intraoperative ultrasound navigation in HBP surgery started in September 2024, with data currently being collected from four institutions including ours.
Multicenter Collaborative Research
We are also collaborating with the Graduate School of Pharmaceutical Sciences at the University of Tokyo on a project evaluating cost-effectiveness in cancer care, including QOL-based economic assessments for HBP cancers. The initial results will be presented at domestic conferences, and a manuscript is in preparation.
Ongoing Clinical Trial Participation
- JCOG1315C: Non-randomized comparison of proton beam therapy versus surgical resection for resectable hepatocellular carcinoma
- JCOG2101C: Phase III trial comparing preoperative gemcitabine + S-1 vs. gemcitabine + nab-paclitaxel in elderly patients with resectable pancreatic cancer
- JCOG2202: Phase III non-inferiority trial of laparoscopic versus open distal pancreatectomy for resectable pancreatic cancer
- COSMOS trials: COSMOS-PC, COSMOS-HCC, COSMOS-BTC
- Studies on adhesion-prevention materials in planned two-stage hepatectomy
- International retrospective study of non-traumatic emergency pancreaticoduodenectomy
- Multicenter study on novel prognostic indicators in hepatocellular carcinoma
Education
Each resident attends major HBP surgeries once or twice a week, mainly as a first assistant. Depending on their skill, they also have the opportunity to act as the primary operator. For each case, they learn how to decide on the indication and the type of procedure based on the preoperative images. In the operating room, the residents learn not only each step of HBP surgery but also tips on how to safely perform the surgery. Through two years of training, chief residents perform highly difficult HBP surgeries and aim to become board-certified expert surgeons (Japanese Society of Hepato-Biliary-Pancreatic Surgery) or endoscopic surgical skill qualified surgeons (Japan Society for Endoscopic Surgery). They may also conduct research for a year in the research institute. Motivated residents also have the opportunity to make presentations in academic meetings and write academic papers in English. Visitors from both domestic and foreign institutions are welcome anytime.
Future Prospects
HBP malignancy often requires technically demanding and invasive surgical procedures; however, its long-term prognosis is not yet satisfactory. Our most important mission is to establish safer and more feasible surgical techniques, including perioperative patient management, and to promote survival outcomes through multidisciplinary approaches. Owing to the recent advances in chemotherapy, we have achieved curative surgical resection for some of our patients with initially unresectable pancreatic cancer due to local advancement. We will therefore prospectively assess the feasibility of conversion therapy.
Minimally invasive surgical treatments with laparoscopic and robot-assisted surgery have been established for selected patients with low-malignant pancreatic tumors or primary/metastatic liver cancers that are not only peripherally located but also centrally located. We started to extend the indication of minimally invasive surgery for patients with more aggressive diseases and those undergoing repeat surgery.
We will continue to strive to create new skills and treatment strategies. We also expect to perform clinical trials to explore unclarified clinical questions.
List of papers published in 2024
Journal
1. Hirose S, Ban D, Matsui Y, Mizui T, Miyata A, Nara S, Esaki M. Laparoscopic liver resection with retroperitoneoscopy for the treatment of right dorsal liver tumors (with video). Surgery today, 55:723-726, 2025
2. Takamoto T, Nara S, Ban D, Mizui T, Mukai M, Esaki M, Shimada K. Chronological evolution in liver resection for hepatocellular carcinoma: Prognostic trends across three decades in early to advanced stages. European journal of surgical oncology, 51:109461, 2025
3. Murase Y, Esaki M, Mizui T, Takamoto T, Nara S, Ban D, Hiraoka N, Shimada K. Optimal lymph node dissection area for pancreatic neuroendocrine neoplasms by tumor location, size, and grade. Surgery, 180:109029, 2025
4. Tsukamoto F, Tsukamoto S, Kato T, Nagata H, Takamizawa Y, Moritani K, Kinugasa Y, Esaki M, Kanemitsu Y, Igarashi A. Cost-effectiveness analysis of postoperative surveillance for stage IV colorectal cancer in Japan: An economic modeling study. Ann Gastroenterol. Surg, 0:1-9, 2025
5. Sakamoto S, Hiraide H, Minoda M, Iwakura N, Suzuki M, Ando J, Takahashi C, Takahashi I, Murai K, Kagami Y, Mizuno T, Koike T, Nara S, Morizane C, Hijioka S, Kashiro A, Honda K, Watanabe R, Urano Y, Komatsu T. Identification of activity-based biomarkers for early-stage pancreatic tumors in blood using single-molecule enzyme activity screening. Cell reports methods, 4:100688, 2024
6. Takayama Y, Tsukamoto S, Kudose Y, Takamizawa Y, Moritani K, Esaki M, Kanemitsu Y, Igarashi A. Cost-effectiveness of surveillance intervals after curative resection of colorectal cancer. Japanese journal of clinical oncology, 54:637-646, 2024
7. Hijioka S, Yamashige D, Esaki M, Honda G, Higuchi R, Masui T, Shimizu Y, Ohtsuka M, Kumamoto Y, Katanuma A, Gotohda N, Akita H, Unno M, Endo I, Yokoyama Y, Yamada S, Matsumoto I, Ohtsuka T, Hirano S, Yasuda H, Kawai M, Aoki T, Nakamura M, Hashimoto D, Rikiyama T, Horiguchi A, Fujii T, Mizuno S, Hanada K, Tani M, Hatori T, Ito T, Okuno M, Kagawa S, Tajima H, Ishii T, Sugimoto M, Onoe S, Takami H, Takada R, Miura T, Kurita Y, Kamei K, Mataki Y, Okazaki K, Takeyama Y, Yamaue H, Satoi S. Factors Affecting Nonfunctioning Small Pancreatic Neuroendocrine Neoplasms and Proposed New Treatment Strategies. Clinical gastroenterology and hepatology, 22:1416-1426.e5, 2024
8. Umino R, Nara S, Mizui T, Takamoto T, Ban D, Esaki M, Hiraoka N, Shimada K. Impact of Surgical Margin Status on Survival and Recurrence After Pancreaticoduodenectomy for Distal Cholangiocarcinoma: Is Microscopic Residual Tumor (R1) Associated with Higher Rates of Local Recurrence? Annals of surgical oncology, 31:4910-4921, 2024
9. Umino R, Nara S, Mizui T, Takamoto T, Ban D, Esaki M, Hiraoka N, Shimada K. ASO Author Reflections: Future Perspectives in Surgical Management of Distal Cholangiocarcinoma: Insights from Surgical Margin Status and Recurrence Patterns. Annals of surgical oncology, 31:4946-4947, 2024
10. Yamamoto Y, Sugiura T, Esaki M, Takahashi Y, Arita J, Hashimoto M, Sakamoto Y, Konishi M, Sano T, Notsu A, Uesaka K, Shimada K. Impact of biliary drainage method before pancreaticoduodenectomy on short- and long-term outcomes in patients with periampullary carcinoma and obstructive jaundice: A multicenter retrospective analysis. Surgery, 176:616-625, 2024
11. Okano N, Kawai M, Ueno M, Yu X, Inoue Y, Takahashi S, Wang W, Takahashi H, Okamura Y, Morinaga S, Matsumoto I, Shimizu Y, Yoshida K, Yamamoto T, Ohtsuka M, Inokawa Y, Nara S, Tamura J, Shinoda S, Yamamoto K, Yamaue H, Furuse J. Outcomes of patients with initially unresectable pancreatic cancer who underwent conversion surgery after FOLFIRINOX or gemcitabine plus nab-paclitaxel chemotherapy: A multicenter retrospective cohort study (PC-CURE-1). Journal of hepato-biliary-pancreatic sciences, 31:816-829, 2024
12. Hirono S, Higuchi R, Honda G, Nara S, Esaki M, Gotohda N, Takami H, Unno M, Sugiura T, Ohtsuka M, Shimizu Y, Matsumoto I, Kin T, Isayama H, Hashimoto D, Seyama Y, Nagano H, Hakamada K, Hirano S, Nagakawa Y, Mizuno S, Takahashi H, Shibuya K, Sasanuma H, Aoki T, Kohara Y, Rikiyama T, Nakamura M, Endo I, Sakamoto Y, Horiguchi A, Hatori T, Akita H, Ueki T, Idichi T, Hanada K, Suzuki S, Okano K, Maehira H, Motoi F, Fujino Y, Tanno S, Yanagisawa A, Takeyama Y, Okazaki K, Satoi S, Yamaue H. Is multidisciplinary treatment effective for invasive intraductal papillary mucinous carcinoma? Annals of gastroenterological surgery, 8:845-859, 2024
13. Ito S, Takamoto T, Nara S, Ban D, Mizui T, Nagata H, Takamizawa Y, Moritani K, Tsukamoto S, Kanemitsu Y, Kinugasa Y, Esaki M. RAS mutation associated with short surgically controllable period in colorectal liver metastases: a retrospective study. World journal of surgical oncology, 22:247, 2024
14. Uemura S, Ban D, Esaki M, Nara S, Takamoto T, Mizui T, Shimada K. Risk factor analysis of postoperative pancreatic fistula after distal pancreatectomy with a focus on the peritoneum to portal vein distance on computed tomography. World journal of surgery, 48:2496-2504, 2024
15. Baba H, Oba A, Tanaka K, Miura T, Ban D, Edanami M, Ishikawa Y, Ohgi K, Tanaka H, Shintakuya R, Ikenaga N, Ijichi T, Kiya Y, Muranushi R, Yamaki S, Miyazaki N, Takeuchi S, Aoki S, Mizui T, Tanaka M, Ueda H, Dei H, Takami H, Okada K, Nakata K, Mataki Y, Osakabe H, Shibuya K, Hashimoto D, Inoue Y, Hirano S, Unno M, Esaki M, Kitago M, Akahoshi K, Sugiura T, Ebata T, Uemura K, Nakamura M, Otsuka T, Nagakawa Y, Fujii T, Satoi S, Takahashi Y. The efficacy of wrapping with polyglycolic acid mesh and fibrin glue in preventing clinically relevant pancreatic fistula after minimally invasive distal pancreatectomy (WRAP Study): study protocol for a multicenter randomized controlled trial in Japan. BMC surgery, 24:314, 2024
16. Yoshino J, Nara S, Yokoyama M, Ban D, Mizui T, Miyata A, Esaki M. Prognostic impact of lymph node dissection in intrahepatic cholangiocarcinoma: a propensity score analysis. Langenbeck's archives of surgery, 410:3, 2024
17. Komachi MH, Kamibeppu K. Association between family functioning, resilience, and psychosocial burden among family members of patients in the intensive care unit: A cross-sectional study. Journal of International Nursing Research, 2:e2022-0032, 2023
