Annual Report 2024
Department of Radiological Technology
I.Radiological Diagnosis
Hiroshi Tanizaki, Kanyu Ihara, Toshihiro Ishihara, Atsushi Urikura, Hirobumi Nagasawa, Naoya Ikeno, Jun Torii, Ryouta Haga, Naoki Ikari, Misayo Seki, Satomi Yamamoto, Tatsushi Komori, Naoya Kamisaka, Makoto Mimatsu, Jun Shishido, Hiromi Suzuki, Minami Maruyama, Eiko Taguchi, Yuya Kanai, Ryo Kawana, Yusuke Wakatsuki, Nao Ozaki, Yuhei Shimizu, Seiya Sato, Akira Yoshida, Seiya Mochizuki, Chihiro Ishiyama, Aya Shimoike, Satsuki Watanabe, Ayame Sugo, Kazuki Matsubara, Takumi Miyairi, Yuki Tsunoda, Yutaro Tsukahara, Kazuki Takaso, Yuuki Thunoda, Ryutaro Zenbayashi, Ryo Hosono, Yoshiki Ishihara, Kaho Miyagi, Madoka Hasegawa, Mio Kakinoki, Chihiro Ishiyama, Banri Shinozaki, Maho Sunaga, Saya Sakurai, Aika Miura, Yu Terafuji, Kana Endo, Ren Kuroda, Miho Kikuchi, Ryo Takahashi, Ami Tushara, Taisei Miyakoshi, Ami Nakaie, Yukiko Nagawa
Introduction
The Department of Radiological Technology makes full use of the technology to provide precise medical images for patients. Human resource development of radiological technologists has always been, and continues to be, a theme in our department. We accept and educate residents in radiological technology.
The Team and What We Do
The National Cancer Center Hospital has diagnostic imaging devices as shown in Table 1. We performed a total of 160,915 examinations as shown in Table 2 in FY2024.
Table 1. Number of diagnostic imaging devices

Table 2. Number of examination cases in FY2024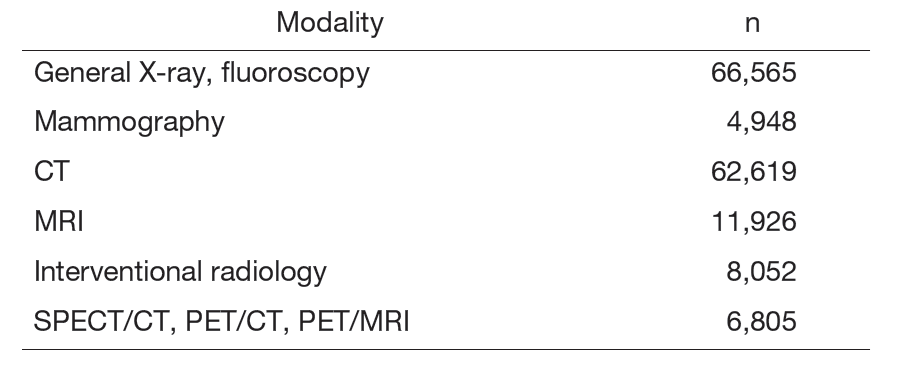

Research Activities
The radiography team analyzed the causes of retakes, updated standards, supported junior staff, and improved quality using the PDCA cycle.
The mammography team adjusted imaging settings to capture dense breasts within DRLs 2020 limits and established proper imaging conditions.
The CT division provided both qualitative and quantitative value-added diagnostic information by leveraging deep-learning-based image reconstruction, iodine mapping, and virtual monochromatic imaging. In parallel, we implemented multiple workflow-optimization initiatives, including presetting selected RIS input items, consolidating CT colonography examinations onto designated scanners, redistributing out-of-slot CT orders, and increasing the number of scanners operating during the lunch hour by reorganizing staff assignments. These measures led to improvements in both the quality and efficiency of clinical services.
In addition, as part of our academic activities, we presented our work on assessing the depth of invasion in tongue cancer using ultra-high-resolution CT at an international conference, where its potential for clinical application received high recognition.
The MRI team introduced a handheld ferromagnetic detector and validated its sensitivity and usability in daily operations. These efforts strengthened safety management and improved examination reliability.
The IVR team promoted interdisciplinary collaboration and supported diagnosis and treatment with 3D simulation images and an app was developed with industry partners to track embolic materials and overlay puncture paths. A working group was formed to reduce material costs.
The gastrointestinal team focused on staff training due to fewer esophageal X-rays. The endoscopic X-ray team improved safety through room upgrades, better information sharing, case conferences, and emergency drills.
The RI team completed PET/CT installation, improving image quality and exam efficiency. Legal steps were taken to replace another unit, and a new radionuclide therapy for unresectable PPGL was introduced.
Clinical Trials
To establish a system for disclosing and sharing medical radiation doses with patients, a software-based dose management system was developed.
In collaboration with Komazawa University, a survey was conducted to assess the competencies and literacy of radiological technologists regarding radiation disasters.
As part of a joint research project on deep learning-based image processing software for X-ray CT images, image quality was evaluated using phantom studies.
A study was conducted on the number of X-ray CT scanners, population, and medical resources in Japan, revealing regional disparities in CT scanner distribution and their correlation with population and healthcare availability.
Education
- During conferences within the radiological diagnosis department, each technologist gave lectures on their area of expertise, contributing to skill development.
- To improve research skills among beginners, academic research seminars were held regularly.
- Multisite radiology conferences have been continuously held with cancer treatment core hospitals across Japan, effectively facilitating inter-facility information sharing on radiological techniques.
- Hospital trainees were accepted from Juntendo University, International University of Health and Welfare, Tokyo Metropolitan University, Kyorin University, Komazawa University, and Tsukuba International University. Table 3 shows the results of accepted contracted training and practical training.
- Accepted voluntary training in the radiation therapy department from Tokyo Jikei University Hospital and NHO Tokyo Medical Center
- Accepted voluntary training in the diagnostic radiology department from NHO Fukuyama Medical Center.
- We conducted personnel exchanges with Tokyo University Hospital to provide mutually enriching education.
- We conducted personnel exchanges with Kyoto University Hospital to provide mutually enriching education.
- The 21st Academic Exchange Meeting on Advanced Radiation Science and Technology was held jointly with the University of Tokyo Hospital and Kyoto University Hospital.
Table 3. Results of contracted training andpractical training 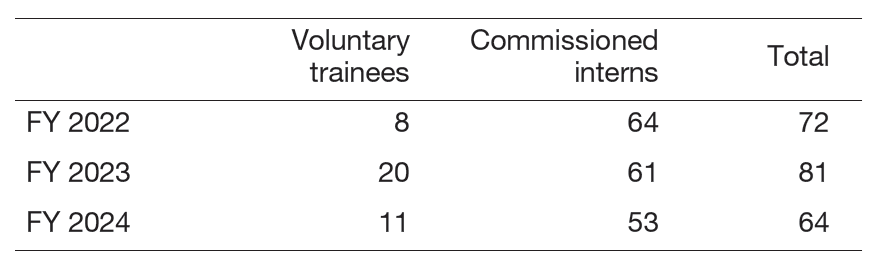 ">
">
 ">
">
Future Prospects
The Department of Radiological Technology has established a residency program for radiological technologists beginning in FY2022. We will continue to provide ongoing education for technologists specializing in cancer medicine.
List of papers published in 2024
Journal
1. Aoyama T, Koide Y, Shimizu H, Urikura A, Kitagawa T, Hashimoto S, Tachibana H, Kodaira T. A cross-national investigation of CT, MRI, PET, mammography, and radiation therapy resources and utilization. Japanese journal of radiology, 43:109-116, 2025
2. Mukaigawa T, Asakura K, Tsuzuki A, Urikura A, Yoshida T, Goto S, Okada S, Hiiragi Y, Sato F. Subtraction CT Improves Detectability of Mandibular Bone Invasion in Oral Squamous Cell Carcinoma. The Laryngoscope, 135:1706-1714, 2025
3. Takiguchi K, Urikura A, Yoshida T, Nakashima K, Asakura K, Endo M. Computed tomographic pulmonary angiography using low tube voltage and slow contrast medium injection. Emergency radiology, 32:369-376, 2025
4. Urikura A, Ishii I, Sone M, Sugawara S, Itou C, Kimura S, Suzuki H, Ishihara T, Kusumoto M. Preliminary phantom study of four-dimensional computed tomographic angiography for renal artery mapping: Low-tube voltage and low-contrast volume imaging with deep learning-based reconstruction. Radiography (London, England : 1995), 31:102929, 2025
5. Higuchi Y, Watanabe T, Tabeta A, Yamana H, Tanaka Y, Tsutsumi Y. Diagnostic Accuracy of Dual-Energy Computed Tomography for Bowel Necrosis in Acute Abdomen With Bowel Ischemia. Cureus, 17:e81057, 2025
6. Watanabe S, Urikura A, Ohashi K, Kitera N, Tsuchiya T, Kasai H, Kawai T, Hiwatashi A. Artifact reduction in low and ultra-low dose chest computed tomography for patients with pacemaker: A phantom study. Radiography (London, England : 1995), 30:770-775, 2024
7. Yoshida T, Urikura A, Endo M. Vendor-Specific Correction Software for Apparent Diffusion Coefficient Bias Due to Gradient Nonlinearity in Breast Diffusion-Weighted Imaging Using Ice-Water Phantom. Journal of computer assisted tomography, 48:889-896, 2024
